Maggie Teichmann – The Life of a Child Life Specialist. It’s more than playing games
Child Life specialist Maggie Teichmann talks about what it means to her to be able to help patients and families.
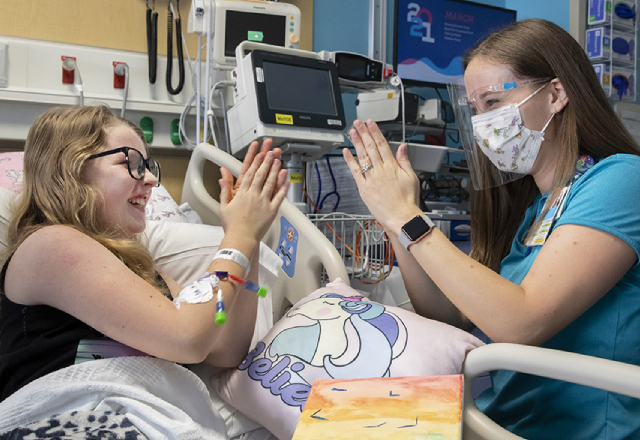
Maggie Teichmann is a Child Life specialist in the pediatric intensive care unit at Johns Hopkins All Children's.
Maggie Teichmann got her first taste of a Child Life program as a 9-year-old at Vanderbilt Children’s Hospital in Nashville, Tennessee. “My youngest brother was about to turn 1, and he was admitted into the PICU (pediatric intensive care unit) for brain surgery. During his time in the hospital, a Child Life specialist helped my family celebrate his first birthday. I was able to help plan it at the hospital and it had such a positive impact on my family during a time where we were so terrified. She gave us a glimpse of hope and joy during that scary time.”
“At that point, I did not know she was a Child Life specialist, but I knew that someone had impacted my parents, my siblings, and myself in such a positive way. I knew from that point forward that I wanted to work with children and families in the hospital.”
“Today my brother is 19-years-old, and he fully recovered.”
When it came time to attend college and select a career, Maggie still remembered the experience she had with her brother’s hospitalization. She attended college at the University of Tennessee at Chattanooga and received a degree in Child and Family Studies. Post-graduation, she required a 600-hour Child Life internship at Wolfson’s Children’s Hospital in Jacksonville, Florida. Once that was completed, she took an extensive exam and soon became a Certified Child Life Specialist.
“When I tell people outside the hospital what I do, many times they have never heard of child life. We help patients and families cope with the stressors and uncertainties of hospitalization. Our goal is to reduce fear, anxiety, and pain through therapeutic play, preparation and education. When I speak to a child, I say I am like a teacher, I help answer and explain all of their questions about the hospital. I’m also much like a coach, providing encouragement and support alongside patients and families in the ICU. And I save the best for last, I am like a “Play Lady,” I help make the hospital more fun with toys, games, arts and crafts.”
What brought you to Johns Hopkins All Children’s Hospital?
Right after I got married, my husband got a job that brought us to the Tampa Bay area. I soon joined Johns Hopkins All Children’s Hospital in 2020 as a Certified Child Life Specialist in the PICU. It was my dream job. Because of the past life experiences I mentioned, the PICU has always had a special place in my heart. It’s kind of a full circle for me. It’s very special.
What’s a normal day look like for you?
I start seeing my kids after rounds have been completed. My work can involve anything from teaching a patient about a new medical diagnosis to normalizing their day by implementing play into their schedule. Other interventions may include: preparation and support for a procedure, providing sibling support, engaging in therapeutic activities, supporting through bereavement, or providing active listening and emotional support to caregivers. Many caregivers enjoy co-treating and being involved as we create a game plan and coping strategies for their kids to succeed best.
There are so many ups and downs when working with hospitalized children. Everyday there are children who are able to leave the PICU, breathe on their own, or even take their first lap around the unit after a tough admission. It is such a blessing being able to witness how resilient our patients can be, but I have found that it’s still an honor to be a part of the hard days too. Interactions with patients and families might not always go as planned, a new illness could be diagnosed, a family may have to say goodbye to their child or sibling. All of these ups and downs in the PICU can be difficult, but at the end of the day, I feel blessed to be able to work alongside of them throughout their journey.
I feel so fortunate to work here. I’ve been involved with other Child Life programs, but this one is just spectacular. Our Child Life department is a tight-knit group that all prioritizes family-centered care. It is inspiring to be surrounded by so many people who all want the best for our families.
How has technology changed the job of a Child Life specialist?
We still use puppets to teach kids about medical procedures, but we also use iPads a lot. It’s especially helpful during procedures. Using the iPad helps divert their attention away from the procedure, and it’s also beneficial for kids who need visual preparation for an upcoming procedure.
An example would be preparing a patient for a PICC line (a thin, soft, long catheter (tube) that is inserted into a vein in a child's arm, leg or neck. It is used for long-term intravenous (IV) antibiotics, nutrition or medications, and for blood draws). They are able to see what it looks like, where it will be on their body, how it functions, and what to expect during placement. Prepping with the iPad gives patients a good visual of what they will see and experience, it clears up misconceptions, and allows them to gain control of their situation by knowing what to anticipate.
We have to adjust our teaching strategies all throughout the day since we work with infants to adolescents. Child Life specialists are educated on how to assess a patient appropriately based off their age and developmental level so that we can best help them specifically to their hospitalization. What I share with younger children verses older kids is totally different, but thankfully our technology can adapt to all ages.
How has COVID-19 impacted your work?
It’s definitely more difficult for our families due to the restrictions that limited one caregiver allowed at bedside. It’s also hard for the patients in the designated COVID-19 area. I am not allowed to go into those rooms, so a lot of my interactions are done on the other side of the glass door. I make it a goal to do the same interventions for those patients as I would do for those in person. Unfortunately, introducing services over the phone is not the same, but pairing it with a big wave from the other side of their glass door is a little more fun and personable.
Luckily, our Child Life activity techs have been implementing more live broadcasts on our Get Well Network, so patients are able to virtually participate in game shows and activities with each other. I see more and more kids positively impacted by this change due to COVID-19. It’s truly their favorite part of the week.
What do you do in your spare time?
I go to a lot of basketball games since my husband is the men’s basketball coach at Florida College in Temple Terrace. He had a winning season this year, so that was fun. I also help with the volleyball team at the same college, so most of our free time is hanging out at the gym during season. Since we are from Tennessee, we have really enjoyed taking advantage of the nice Florida beaches.
What makes you smile at the end of the day?
I feel like I am smiling all throughout the day. It is surreal that I am living out my dream job and I feel so fortunate to be the Child Life specialist in the PICU. The patients in this population give me so much joy and I love working together with the PICU staff to support them. As I mentioned earlier, there are many positive and difficult things that our families may endure, but I feel as if my bucket is filled at the end of each day, and I am able to leave here with a smile on my face after seeing how strong these kiddos are.
