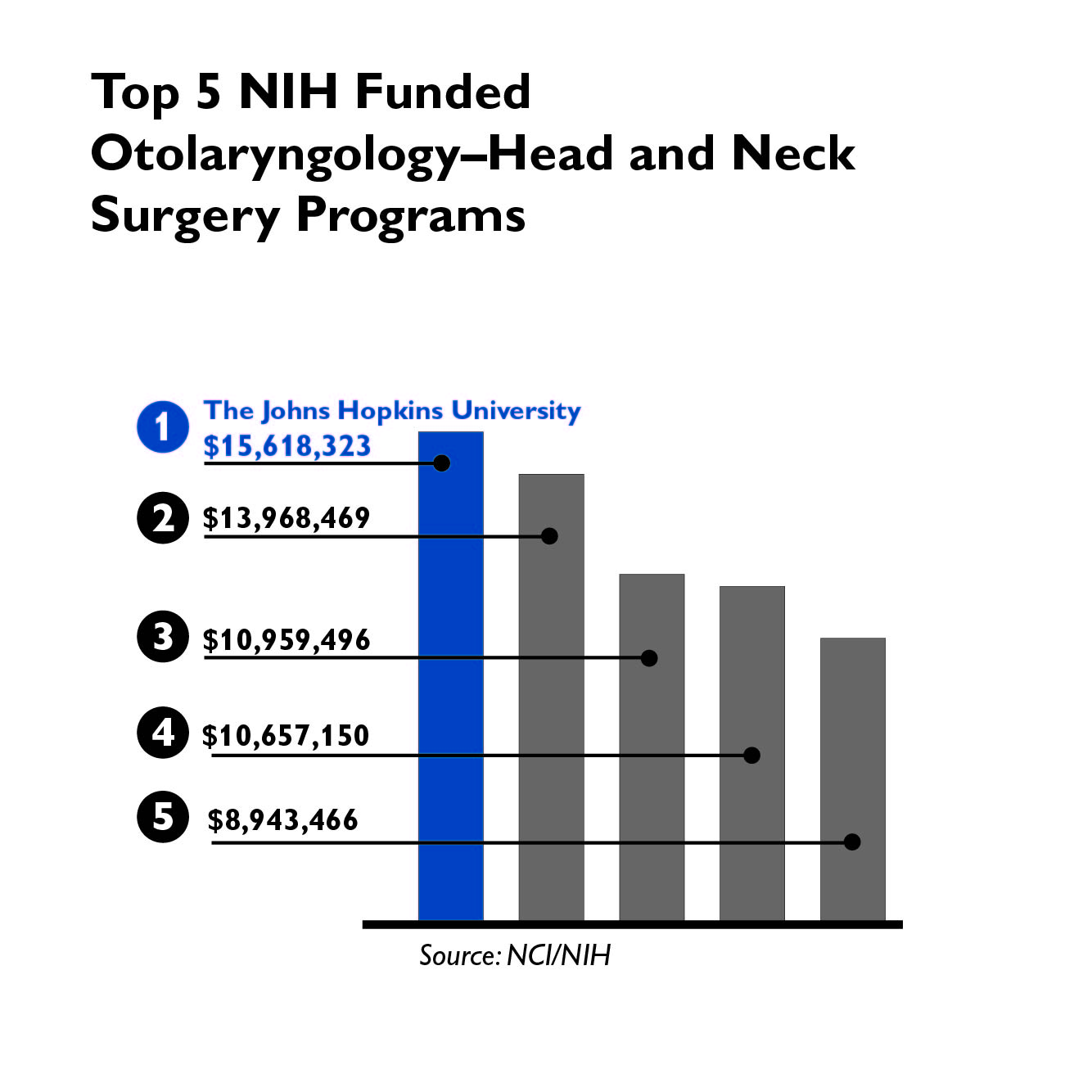
The Johns Hopkins Department of Otolaryngology–Head and Neck Surgery continued to innovate in the areas of patient care and clinical research throughout 2020 despite the challenges of the pandemic — which included the redeployment of approximately 20 employees to positions across The Johns Hopkins Hospital and the Johns Hopkins University School of Medicine.
A clinical trial for a new type of vestibular implant — a device based on technology developed at Johns Hopkins to treat bilateral vestibular hypofunction (BVH) — showed that participants experienced improvements in posture, gait and patient-reported outcomes. By surgically implanting a stimulator that electrically bypasses malfunctioning areas of the inner ear, surgeons can help partially restore patients’ sensation of balance. “Participants in this trial are true pioneers — the first to use a vestibular implant as a long-term, 24-hour-per-day sensory restoration treatment,” says Charley Della Santina, senior author of the study, director of the Johns Hopkins Cochlear Implant Center, and professor of otolaryngology–head and neck surgery and biomedical engineering at the Johns Hopkins University School of Medicine.
In the past year, Johns Hopkins clinicians also began regularly offering radiofrequency ablation (RFA) to treat thyroid nodules. Although RFA has been used for decades for conditions affecting the heart, liver and other areas, its use in the neck was limited due to the close proximity of vulnerable anatomical structures. With increasingly refined techniques and improved technology, RFA has become a popular treatment for benign thyroid nodules in various parts of the world. In late 2019, Johns Hopkins pioneered use of the technique in the U.S. Otolaryngologist–head and neck endocrine surgeons Jonathon Russell and Ralph Tufano and colleagues offer the procedure, which, depending on the nodule’s size, can take as little as 30 minutes, with damaged tissue disappearing as quickly as a few weeks.
The department also introduced state-of-the-art treatment pathways for patients with head and neck cancer, and combined appointments so these patients can see a multidisciplinary team during a single visit. “Now our patients with cancer are seen by medical oncology, radiation oncology and speech-language pathology in an efficient way,” says Carole Fakhry, otolaryngologist–head and neck surgeon and director of the Johns Hopkins Head and Neck Cancer Center.
Also during the pandemic, the Johns Hopkins Swallowing Center expanded services to the Johns Hopkins Outpatient Center, the Johns Hopkins Health Care and Surgery Center in Green Spring Station and Suburban Hospital. The center also began offering new procedures, including transnasal esophagoscopy at the Health Care and Surgery Center. Laryngologist Shumon Dhar and colleagues use the technique to examine the esophagus and stomach with an ultrathin endoscope inserted through the nose. The approach can be combined with other diagnostic and therapeutic procedures.
When appropriate, surgeries for the sinus, the thyroid, cochlear implants, pediatrics and facial plastics transitioned to the Green Spring Station Health Care and Surgery Center to support expansion of capacity at The Johns Hopkins Hospital for patients with COVID-19. The moves also provided peace of mind for patients concerned about COVID-19 in a hospital setting. The department increased its use of telemedicine too, completing nearly 7,000 visits in 2020, compared with just five the year before.