Discoveries Timeline
-
1982 (Document) :
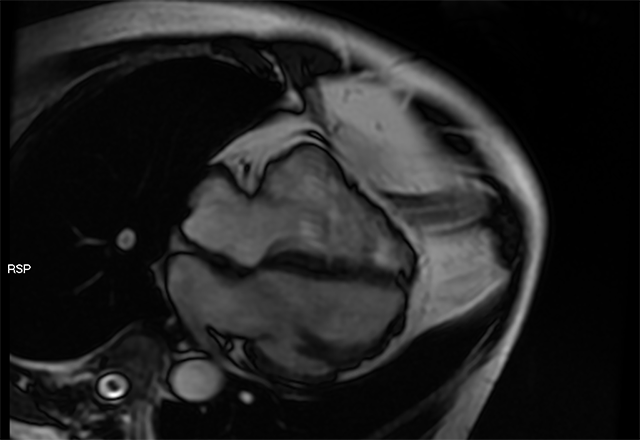
Arrhythmogenic right ventricular dysplasia (ARVD) is first defined as a slowly progressive heart disease in modern scientific literature by French and American physicians. In the condition, fat and scar tissue replaces damaged heart tissue in the right ventricle and disrupts the normal heart rhythm.
-
1988 (Document) :
Physicians at the University of Padua, Italy, describe arrhythmogenic right ventricular cardiomyopathy (ARVC) in young people who died from sudden cardiac death. A group of these patients died while exercising, suggesting the link between ARVC and exertion.
-
1994 (Document) :
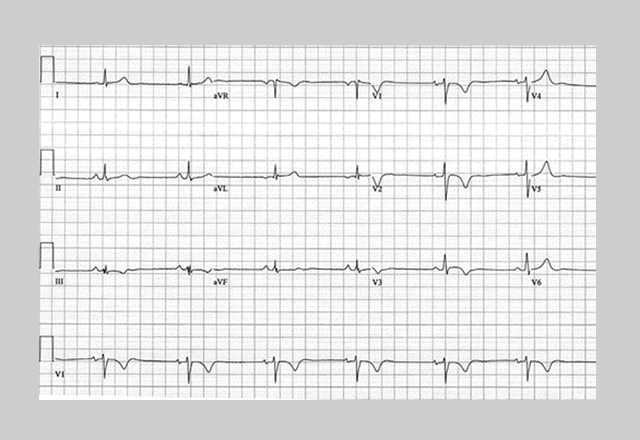
The first ARVC diagnostic criteria is published by an international team of physicians. The team shows that people with ARVC have irregular heart rhythms when exercising or during times of emotional stress.
-
1999 (Document) :
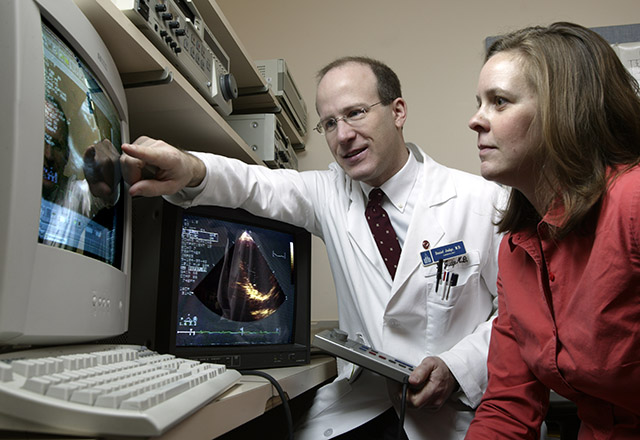
Johns Hopkins Medicine launches the Arrhythmogenic Right Ventricular Dysplasia (Cardiomyopathy) Program and establishes a patient registry.
-
2000 (Research) :
Researchers from Greece and the United Kingdom find the first ARVC risk gene junction plakoglobin (JUP). The gene codes for the plakoglobin protein which helps anchor heart muscle cells in place to one another.
-
2002 (Document) :
The North American ARVC Registry is established. Johns Hopkins radiologist David Bluemke runs the MRI Core Lab, and Johns Hopkins is the leading enrolling center.
2002 (Document) :
A new ARVC risk gene desmoplakin (DSP) is identified by physicians at the University of Padua, Italy. The protein desmoplakin made by this gene is, like plakoglobin (JUP), found in the machinery that helps heart tissue cells stick to one another.
-
2005 (Document) :
The first major publication from the Johns Hopkins registry describes outcomes of 100 U.S. ARVC patients. Of the 66 patients still alive, 44 have implantable defibrillators, five have signs of heart failure and two have heart transplants. Sudden cardiac death had killed 23 of the patients.
-
2004 - 2006 (Research) :
The remaining ARVC risk genes that play a role in heart cell connections are identified: plakophilin 2 (PKP2) by German researchers, desmocollin 2 (DSC2) by United Kingdom researchers and desmoglein 2 (DSG2) by Daniel Judge at Johns Hopkins.
-
2005 - 2006 (Research) :
Mutations in the plakophilin 2 (PKP2) gene are shown to be the primary reason behind inherited ARVC. These research studies by Dutch, United Kingdom and Johns Hopkins researchers establish the risk in families.
-
2006 (Research) :
-
2010 (Document) :
The ARVC diagnostic criteria is revised and published by worldwide experts including Hugh Calkins, Hari Tandri and David Bluemke of Johns Hopkins. The new criteria include how to use cardiac MRI to visualize the heart, electrocardiograms to measure the heart’s electrical activity and genetic testing.
-
2013 (Document) :
The first human study is published by Cindy James and Hugh Calkins of Johns Hopkins. It demonstrates that exercise increases the likelihood that you will go on to develop ARVC if you have one of the risk genes. They also find that exercise increases heart damage and irregular heartbeats in carriers of ARVC risk genes.
-
2015 (Document) :
The biggest natural history study of ARVC, including 1,001 patients and family members, is published by Johns Hopkins and Dutch research teams using the Dutch and U.S. ARVD registries. This is the first comprehensive study to date that looks at genetic mutations and symptoms combined.
2015 (Document) :
The first comprehensive ARVC-focused treatment guidelines are published by an international task force. These recommendations rank diagnostic measures and treatments based on the amount of scientific evidence backing their support, suggesting lifestyle changes, potential medications and other therapies to prevent irregular heart rhythms.
-
2016 (Research) :
Johns Hopkins creates a mouse model of ARVC. This one contains a mutation in the gene desmoglein 2 (DSG2). Exercise accelerates disease in these mice.
2016 (Document) :
Research teams from Johns Hopkins and University Medical Center Utrecht, Netherlands, clarify family screening methods for ARVC.
-
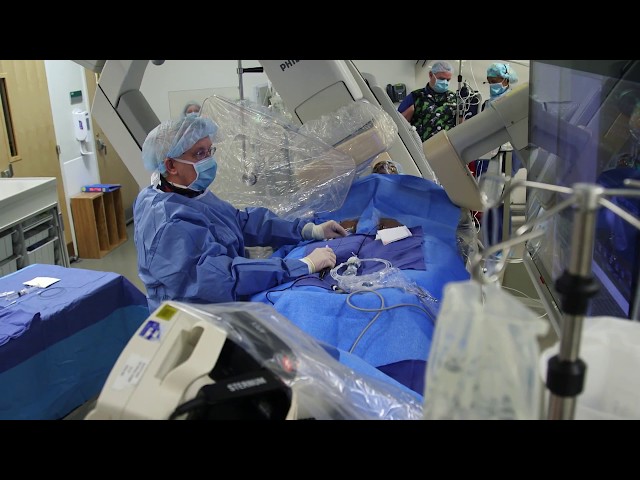
2017 (Video) :
Johns Hopkins’ ARVD/C program becomes a Johns Hopkins inHealth Precision Medicine Center of Excellence .
-
2019 (Document) :
In partnership with the University of Rochester, Johns Hopkins begins the first U.S. clinical trial for a medication to treat ARVC.
2019 (Document) :
A Johns Hopkins team develops a computer program to predict whether a patient with ARVC is at risk of sudden cardiac death and would benefit from an implantable defibrillator.
2019 (Document) :
Find out about the latest research on ARVC/D at Johns Hopkins.