Frontotemporal Dementia
What is frontotemporal dementia?
Frontotemporal dementia (FTD), a common cause of dementia, is a group of disorders that occur when nerve cells in the frontal and temporal lobes of the brain are lost. This causes the lobes to shrink. FTD can affect behavior, personality, language, and movement.
These disorders are among the most common dementias that strike at younger ages. Symptoms typically start between the ages of 40 and 65, but FTD can strike young adults and those who are older. FTD affects men and women equally.
The most common types of FTD are:
- Frontal variant. This form of FTD affects behavior and personality.
- Primary progressive aphasia. Aphasia means difficulty communicating. This form has two subtypes:
- Progressive nonfluent aphasia, which affects the ability to speak.
- Semantic dementia, which affects the ability to use and understand language.
A less common form of FTD affects movement, causing symptoms similar to Parkinson disease or amyotrophic lateral sclerosis (Lou Gehrig’s disease).
What causes frontotemporal dementia?
The cause of FTD is unknown. Researchers have linked certain subtypes of FTD to mutations on several genes. Some people with FTD have tiny structures, called Pick bodies, in their brain cells. Pick bodies contain an abnormal amount or type of protein.
What are the risks for frontotemporal dementia?
A family history of FTD is the only known risk for these diseases. Although experts believe that some cases of FTD are inherited, most people with FTD have no family history of it or other types of dementia.
What are the symptoms of frontotemporal dementia?
Symptoms of FTD start gradually and progress steadily, and in some cases, rapidly. They vary from person to person, depending on the areas of the brain involved. These are common symptoms:
- Behavior and/or dramatic personality changes, such as swearing, stealing, increased interest in sex, or a deterioration in personal hygiene habits
- Socially inappropriate, impulsive, or repetitive behaviors
- Impaired judgment
- Apathy
- Lack of empathy
- Decreased self awareness
- Loss of interest in normal daily activities
- Emotional withdrawal from others
- Loss of energy and motivation
- Inability to use or understand language; this may include difficulty naming objects, expressing words, or understanding the meanings of words
- Hesitation when speaking
- Less frequent speech
- Distractibility
- Trouble planning and organizing
- Frequent mood changes
- Agitation
- Increasing dependence
Some people have physical symptoms, such as tremors, muscle spasms or weakness, rigidity, poor coordination and/or balance, or difficulty swallowing. Psychiatric symptoms, such as hallucinations or delusions, also may occur, although these are not as common as behavioral and language changes.
How is frontotemporal dementia diagnosed?
Family members are often the first to notice subtle changes in behavior or language skills. It’s important to see a healthcare provider as early as possible to discuss:
- Symptoms, when they began, and how often they occur
- Medical history and previous medical problems
- Medical histories of family members
- Prescription medicines, over-the-counter medicines, and dietary supplements taken
No single test can diagnose FTD. Typically, healthcare providers will order routine blood tests and perform physical exams to rule out other conditions that cause similar symptoms. If they suspect dementia, they may:
- Evaluate neurological status health including reflexes, muscle strength, muscle tone, sense of touch and sight, coordination, and balance
- Assess neuropsychological status such as memory, problem-solving ability, attention span and counting skills, and language abilities
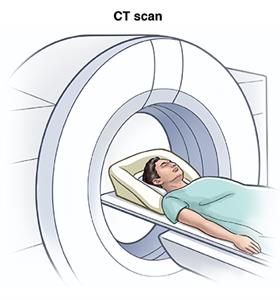
- Order magnetic resonance imaging (MRI) or computed tomography (CT) scans of the brain
How is frontotemporal dementia treated?
Currently, no treatments are available to cure or slow the progression of FTD, but healthcare providers may prescribe medicine to treat symptoms. Antidepressants may help treat anxiety and control obsessive-compulsive behaviors and other symptoms. Prescription sleeping aids can help ease insomnia and other sleep disturbances. Antipsychotic medicine may reduce irrational and compulsive behaviors.
Behavior modification may help control unacceptable or risky behaviors.
Speech and language pathologists and physical and occupational therapists can help adjustment to some of the changes caused by FTD.
What are the complications of frontotemporal dementia?
FTD is not life-threatening ─ people may live with it for years. But it can lead to an increased risk for other illnesses that can be more serious. Pneumonia is the most common cause of death, with FTD. People are also at increased risk for infections and fall-related injuries.
As FTD progressively worsens, people may engage in dangerous behaviors or be unable to care for themselves. They may need 24-hour nursing care or to stay in an assisted living facility or nursing home.
Living with frontotemporal dementia
Coping with FTD can be frightening, frustrating, and embarrassing for the patient and family members. Since some symptoms can’t be controlled, family members shouldn't take their loved one’s behaviors personally. Families need to maintain their own well-being, while ensuring that their loved one is treated with dignity and respect.
Caregivers should learn all they can about FTD and gather a team of experts to help the family meet the medical, financial, and emotional challenges they are facing.
It’s important to find a healthcare provider knowledgeable about FTD. Other healthcare specialists who may play a role on the team are home care nurses, neuropsychologists, genetic counselors, speech and language therapists, as well as physical and occupational therapists. Social workers can help the patient and caregivers find community resources, such as medical supplies and equipment, nursing care, support groups, respite care, and financial assistance.
Attorneys and financial advisors can help families prepare for the later stages of the disease.
Advanced planning will help smooth future transitions for the patient and family members, and may allow all to participate in the decision-making process.
Little solid evidence exists that antioxidants and other supplements help those with FTD. You and your family members should talk with your healthcare provider about whether to try antioxidants and other supplements, such as coenzyme Q10, vitamin E, vitamin C, and B vitamins to support brain health.
When should I call my healthcare provider?
If you are diagnosed with FTD, you and your caregivers should talk with your healthcare providers about when to call them. Your healthcare provider will likely advise calling if your symptoms become worse, or if you have obvious or sudden changes in behavior, personality, or speech. This includes mood changes, such as increasing depression or feeling suicidal.
It can be very stressful for a caregiver to take care of a loved one with FTD. It's normal to have feelings of denial, anger, and irritability. Caregivers may also have anxiety, depression, exhaustion, and health problems of their own. Caregivers should contact their healthcare provider if they have any of these signs of stress.
Key points
- Frontotemporal dementia is a group of disorders characterized by the loss of nerve cells in the frontal and temporal lobes of the brain, which causes these lobes to shrink. The cause of FTD is unknown.
- Symptoms typically first occur between the ages of 40 and 65 and can include changes in personality and behavior, progressive loss of speech and language skills, and sometimes physical symptoms such as tremors or spasms.
- FTD tends to progress over time. Treatments can't cure the disease, but some medicines and other treatments, such as speech therapy can sometimes help with symptoms. If you have FTD, you may eventually need full-time nursing care, or to stay in an assisted living facility or nursing home.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
- Know the reason for your visit and what you want to happen.
- Before your visit, write down questions you want answered.
- Bring someone with you to help you ask questions and remember what your provider tells you.
- At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new instructions your provider gives you.
- Know why a new medicine or treatment is prescribed, and how it will help you. Also know what the side effects are.
- Ask if your condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if you do not take the medicine or have the test or procedure.
- If you have a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your provider if you have questions.