Endometrial Cancer
Reviewed By:
What You Need to Know
- Endometrial cancer starts in the lining of the uterus — the endometrium.
- Being overweight or obese greatly increases a woman’s chance of developing endometrial cancer. Other risk factors include age, family history, a diagnosis of polycystic ovary syndrome and prior use of the breast cancer treatment drug tamoxifen.
- Symptoms include abnormal vaginal bleeding, pain during intercourse, difficult or painful urination, and pain in the pelvic area.
- Endometrial cancer is highly treatable when found early.
.png?h=200&iar=0&mh=360&mw=520&w=200&hash=E8C7D43634560907435FD3759F98A7FF)
What is endometrial cancer?
Endometrial cancer usually only refers to cancer cells that form and grow in the cells lining the uterine cavity, which is the upper part of the uterus. The cervix is at the bottom of the uterus, and cancer cells that develop in this region are a separate type of cancer: cervical cancer. Uterine sarcoma, which is different from endometrial cancer, is a rare type of cancer that can form in the muscular wall of the uterus.
About 66,200 new cases of endometrial cancer are diagnosed each year in the United States, accounting for 3.4% of all new cancer cases.
Endometrial Cancer Symptoms
Endometrial cancer occurs when healthy uterine cells mutate or change. The abnormal cells multiply, grow and do not die like normal cells. If enough of them grow, they may form a tumor and spread to other tissues or other parts of the body around the uterus.
Early signs of endometrial cancer include:
- Abnormal vaginal bleeding, including significant changes in menstrual cycle or bleeding between periods
- Pain in the pelvic area
- Any vaginal bleeding or spotting after menopause
Endometrial Cancer Risk Factors
- Age: Older people are at higher risk of developing this type of cancer.
- Obesity: People who are obese have higher levels of estrogen, which lead to a hormonal imbalance and can overstimulate the cells lining the uterus to grow abnormally.
- Early menstruation or late menopause: People who start menstruation before age 12, or go into menopause later in life than usual, are more likely to develop endometrial cancer. Having more menstrual periods exposes the uterine lining to more estrogen hormones.
- Genetics: A family history of endometrial cancer increases the risk. Lynch syndrome, an inherited colorectal cancer disease, also increases the risk of endometrial cancer.
- Hormonal changes: Changes in the balance of the two main female hormones (estrogen and progesterone) can affect the endometrium, making cancer more likely to develop. Conditions that affect ovulation, such as Polyendocrine Metabolic Ovarian Syndrome (PMOS), obesity and diabetes, can also change hormone levels and heighten a person’s risk. It is important to have regular menstrual cycles, as this is a sign that ovulation is occurring normally. Discuss with your doctor if you do not have regular menstrual cycles.
- Hormone therapy for breast cancer: Taking hormone therapy (tamoxifen) for breast cancer can increase the risk of endometrial cancer. However, the benefits of reducing the chance of breast cancer recurrence might outweigh these risks, so it’s important to discuss it with your doctor.
Obesity and Cancer Risk

Did you know that up to one-third of cancer deaths in women are attributed to excess body weight? Director of Gynecologic Oncology Amanda Fader and oncology dietitian Mary-Eve Brown discuss the correlation between the two. Learn what you can do to reduce your risk.
Endometrial Cancer Diagnosis
Since endometrial cancer typically causes symptoms, doctors can often detect it at an earlier stage, which usually means a better prognosis (chance of recovery).
There are currently no preventive or early detection endometrial cancer screenings. If you have symptoms, a gynecologist may use one or more of these tests to establish the diagnosis:
- Pelvic exams: Your doctor examines the inside of the vagina and the cervix, and looks for abnormalities. The doctor also feels the size and shape of the uterus and ovaries, which can help identify a problem.
- Transvaginal ultrasound: Your doctor inserts a small wand into the vagina, which sends sound waves to view the uterus and ovaries in detail. Doctors can use it to look at the thickness of the uterine lining or to look at tumors inside the uterus. Ultrasounds also detect ovarian cysts or masses.
- Endometrial sampling (biopsy): Your doctor performs a pelvic exam and removes a small amount of tissue from the uterine lining, using a small brush or a flexible tube. Cells are scraped from the endometrium and sent to a pathologist, who will check for cancer cells.
- Pap smear: A Pap smear is not a screening for endometrial cancer, but it sometimes can show signs of an abnormal endometrium. A Pap smear is a sample of cells collected from the cervix to detect cervical cancer.
Types of Endometrial Cancer
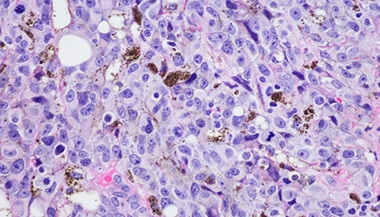
The type of endometrial cancer is determined by how cancer cells look under a microscope.
- Type I endometrial cancer: The most common endometrial cancer is endometrioid adenocarcinoma. These cancer cells are mostly related to estrogen exposure, are less aggressive and have a better prognosis.
- Type II endometrial cancer: These include rarer histologic subtypes, such as serous, clear cell, carcinosarcoma and undifferentiated/dedifferentiated. They tend to grow quickly and are more likely to spread to tissues outside the uterus.
Doctors may also categorize endometrial cancer using molecular subtypes, which provide both predictive and prognostic information. Some common molecular subtype classifications are:
- Copy number high versus low
- p53 mutation status
- Mismatch repair (MMR) protein or microsatellite instability (MSI) status
- DNA polymerase epsilon (POLE) mutation status
- Human epidermal growth factor receptor 2 (HER2) amplification status
Gathering as much information as possible about endometrial cancer cells can help your doctor develop the best treatment plan.
Endometrial Cancer Stages
The stage of endometrial cancer classifies the cancer based on the size of the tumor, whether it has spread to lymph nodes and whether it has metastasized (spread to other parts of the body).
- Stage 1: Cancer cells are present only inside the uterus.
- Stage 2: Cancer cells have spread to the connective tissue of the cervix, but not outside the uterus. No cancer cells are found in nearby lymph nodes.
- Stage 3: Cancer cells have spread to tissues outside the uterus but have not yet reached the rectum or the bladder. Cancer cells may have spread to nearby lymph nodes, the surface of the uterus, ovaries, vagina or tissues in the pelvis.
- Stage 4: Cancer cells have spread to the inner lining of the rectum, the bladder or other areas of the body such as the lungs or liver. Cancer cells may also have spread to distant lymph nodes.
Endometrial Cancer Treatment
Doctors develop a plan to treat endometrial cancer based on several factors, including your:
- Cancer type and stage
- Imaging studies
- Medical history
- Overall health
- Preferences and decisions
Surgery is the most common first step in treating endometrial cancer. Your oncologist may recommend surgery to remove cancer cells or to determine the stage of the cancer and potential need for additional treatment, such as chemotherapy and/or radiation after surgery. Surgery for newly diagnosed endometrial cancer that seems to be early stage typically includes:
- Removal of the uterus, the cervix, bilateral fallopian tubes and ovaries (also known as a total hysterectomy with bilateral salpingo-oophorectomy)
- Lymph node assessment, performed during surgery, which can be done several ways:
- Preoperative and intraoperative assessment to determine if complete removal of pelvic and para-aortic lymph nodes is necessary
- Complete pelvic and para-aortic lymph node dissection
- Sentinel lymph node mapping and biopsy. During this procedure, performed at the time of a hysterectomy, a fluorescent dye is injected into the cervix to map the lymph node channels from the uterus. A special camera helps the surgeon remove the first draining lymph nodes from the site of the primary tumor and determine if cancer has spread to the lymph nodes. Sentinel lymph node mapping allows the surgeon to determine if the cancer has spread to the lymph nodes without removing all lymph nodes.
Your oncologist may recommend additional treatment before or after surgery, including the following.
- Radiation therapy: X-rays or gamma rays that destroy cancer cells
- Chemotherapy: Drugs that target and destroy cancerous cells
- Immunotherapy: Medications that activate the body’s natural ability to find and kill cancer cells
- Hormone therapy: Medications or surgeries that change hormonal activity to stop cancer cell growth or spread
Can I get pregnant with endometrial cancer?
Younger people diagnosed with early stage endometrial cancer may be able to become pregnant in select cases. Patients diagnosed with endometrial cancer who desire fertility-sparing treatment and who meet very specific criteria can be treated with hormonal therapy under the care of a gynecologic oncologist and potentially carry a pregnancy if the cancer responds to treatment. It’s important to discuss your reproductive goals with your oncologist before you begin treatment.
Endometrial Cancer Prognosis
The prognosis for endometrial cancer varies widely by histologic subtype. The most important factor affecting overall survival is stage. The following are the five-year survival rates for patients diagnosed with endometrial cancer.
- Localized: 96% when there is no sign of cancer outside the uterus
- Regional: 72% when the cancer has spread to nearby areas or lymph nodes
- Distant: 20% when the cancer has spread to other distant organs, such as the lungs or liver
Immunotherapy Trial Shows Promise Fighting Endometrial Cancer
Gynecologic cancers can often be difficult to treat, with traditional therapies — surgery, chemotherapy and radiation — becoming less effective with recurrence of disease. Immunotherapy has been showing promise, though, in this area, particularly for endometrial cancer.