Esophageal Cancer Treatment
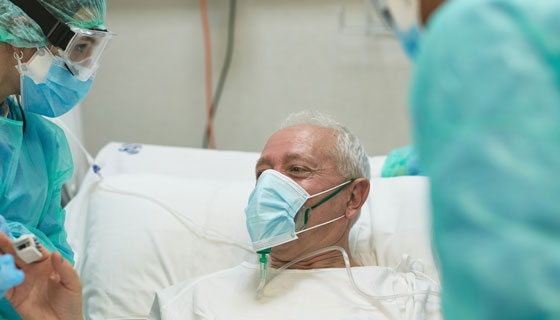
Esophageal cancer develops in the esophagus, which is the tube that connects your throat to your stomach. Most esophageal cancer cases aren’t discovered until they are in advanced stages when immediate treatment is necessary. Treatment options may include:
- Nutrition therapy: Special diets, supplements or intravenous (IV) treatment that build up the body’s strength before cancer treatment begins
- Radiation therapy: The use of X-rays, gamma rays and charged particles to shrink tumors
- Chemotherapy: The use of drugs and other medicines that help the body fight cancerous cells
- Surgery: The removal of cancerous tissue in the esophagus and surrounding areas
- Support services: Additional services such as physical therapy, mental health counseling, and pain management that can help improve your chance of recovery and quality of life during and after treatment
When developing the most effective treatment plan for your unique case, your doctors will consider many factors including:
- The stage of your cancer when it is discovered
- Your overall health and nutrition levels
- The location of the tumor site
- Your personal preferences for different treatment options
Radiation therapy for esophageal cancer
Radiation therapy for cancer treatment, also called radiotherapy, aims to shrink cancerous tumors or lymph nodes. This treatment approach uses high-energy radiation beams to destroy cancer cells.
A radiation oncologist (a doctor who uses radiation to treat cancer) has special expertise in planning customized treatment to effectively shrink the tumor, while sparing healthy tissue near the tumor. Since esophageal cancer tumors are often located near the heart, lungs and main arteries, it is especially important to work with a radiation oncologist who specializes in thoracic (chest) cancer.
Studies have shown that patients experience better results when they receive radiation therapy in esophageal cancer treatment.
- In early-stage cancer, radiation therapy may be the only treatment approach necessary.
- You may also receive radiation therapy before or after surgery, or in combination with chemotherapy.
- Radiation treatments are painless and usually last roughly 15 minutes.
- The main type of radiation therapy used in esophageal cancer treatment is external beam therapy. With external radiation, the patient lies on a table while a radiation therapist directs precisely controlled energy waves directly at the tumor.
- The machine used in external beam therapy is called a linear accelerator. Radiation therapists use advanced treatment planning software to control the size and shape of the machine’s beam to target the tumor while protecting the surrounding healthy tissue.
- Radiation treatments are typically given daily for five to six weeks.
- Patients who have esophageal cancer will most likely receive 25 to 30 treatments (or fractions) of radiation.
- Radiation therapy may cause side effects including nausea, tender skin and fatigue. Your medical team will work with you to manage your pain and other symptoms during your treatment.
Chemotherapy for esophageal cancer
Chemotherapy, or medical oncology, uses powerful drugs to kill cancerous cells and prevent them from coming back. It is one of the most common cancer treatments.
- In most cases, chemotherapy works by interfering with the cancer cells’ ability to grow and reproduce. Immunotherapy, a related treatment, works by strengthening the body’s natural defense systems against cancer.
- Often, treatment for esophageal cancer includes a combination of chemotherapy and radiation therapy before surgery.
- Chemotherapy can cause many side effects like nausea, hair loss and increased risk of infection. Your medical team will work with you to manage pain and any other side effects during your treatment.
Surgery for esophageal cancer
Esophageal cancer surgery requires special expertise because tumors are usually located in the chest, near the heart, lungs and main arteries. Research shows esophageal cancer patients experience better results when they undergo surgery at a center that performs a high number of esophageal cancer surgeries per year.
Types of Esophageal Cancer Surgery
Surgical treatments for esophageal cancer include:
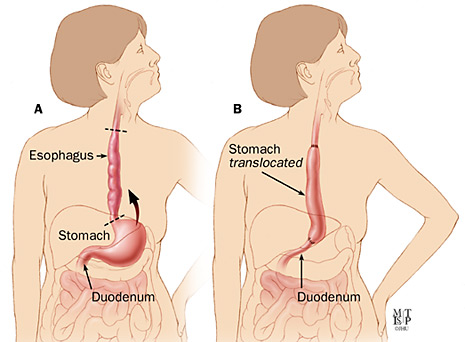
- Transhiatal surgery: In this procedure, the surgeon makes incisions in the neck and abdomen in order to remove the tumor. This approach avoids an incision in the chest but cannot be used if the tumor involves a portion of the stomach or if there are lymph nodes in the chest that must be removed.
- Ivor-Lewis surgery: This approach is most often used when the tumor is located near the stomach or if there are lymph nodes in the chest that need to be removed. The surgeon makes incisions in the abdomen and the right side of the chest.
- Minimally invasive esophagectomy (MIE): In this procedure, the surgeon removes all or part of the esophagus using small incisions for shorter recovery times, less pain and fewer complications than standard esophagectomies, which involve larger incisions.
- Robotic surgery: With this technique, a surgeon performs a robotic esophagectomy (surgical removal of the esophagus) by using robotic arms to manipulate tiny surgical instruments. This minimally invasive approach allows the surgeon a complete range of motion and better precision than other types of surgery.
Combined treatment for esophageal cancer
Most treatment plans for esophageal cancer involve a combined treatment approach, which is when you receive a mix of radiation therapy, chemotherapy or surgery to target cancerous tissue.
- Neoadjuvant therapy is a combination of radiation and chemotherapy that aims to shrink tumors and prevent their reoccurrence before surgery.
- Treating with chemotherapy and radiation together halts the spread of microscopic tumors that have developed beyond the original tumor site.
- Research also shows patients recover more quickly from radiation and chemotherapy when they are performed before surgery rather than after.
Research & clinical trials
Esophageal cancer research and clinical trials allow cancer specialists to explore new approaches to treatment that may benefit patients in the near future. Some areas of research currently underway at Johns Hopkins include:
- Large-scale research on immunotherapy: Immunotherapy is a treatment approach that uses medicines to raise the body’s natural ability to fight cancer patients. Immunotherapy can hold promise for patients who have completed surgery for esophageal cancer but still have cancerous tumors or lymph nodes.
- Biomarkers and chemotherapy: New research on personalized chemotherapy and its applications could be the next frontier in esophageal cancer treatment. By identifying genetic biomarkers that determine how a patient will respond to chemotherapy, doctors can prescribe a course of chemotherapy that is more likely to work for patients with those biomarkers.
- HER2 protein research for esophageal cancer: In breast cancer, chemotherapy drugs target HER2, a protein that responds to treatment with a certain class of drugs. Researchers have found that same protein in esophageal cancer and hope to understand whether esophageal cancer responds to similar treatment.
- Small molecule drug research: Small molecule drugs block the spread of cancer by interfering with specific molecules involved in tumor growth. Researchers are studying the effectiveness of this type of drug therapy on HER2 proteins and other molecules present in esophageal cancer.
- Epigenetic therapy: Epigenetic therapy treats cancer not by killing cancer cells but by reprogramming their patterns of gene expression so that they lose their capacity for uncontrolled growth. By studying the epigenomes of cancer cells, researchers hope to prescribe chemotherapy regimens for esophageal cancer that turn on the genes that fight cancer cells. Researchers are also looking at biomarkers on cancer cells to determine if patients have the kind of genes that would respond to this therapy.
Nutrition therapy for esophageal cancer
Esophageal cancer uniquely affects the body’s ability to receive nutrition normally (through eating and drinking). Many people experience malnutrition and dehydration before receiving an esophageal cancer diagnosis. Your treatment plan might include a phase of healing and building up your body’s strength before tackling the cancer itself.
Dietitians (experts on diet and nutrition) can play an important role throughout your course of treatment. They might prescribe:
- A special diet plan, which takes into consideration any difficulty you may have with swallowing or drinking.
- Intravenous (IV) nutritional therapy, a process that feeds vitamins, minerals, and amino acids directly into the bloodstream through an IV. Sometimes these treatments are also known as “immune drips.”
Patient support services
Esophageal cancer treatment—radiation, chemotherapy and surgery—can be physically and emotionally tiring for patients and their loved ones. Cancer and its treatment can cause exhaustion, malnutrition and other uncomfortable symptoms. After treatment, you may also need assistance to adjust to new habits such as a different way of eating.
There are many types of additional support that are available to esophageal cancer patients, including:
- Nutrition consultations from a registered dietician to address dietary and nutritional needs
- Physical therapy services to help patients who have trouble swallowing or need to gain strength after treatment
- Education in using devices such as a feeding tube or stent, if necessary, to ensure patients are receiving the nutrition they need to recover and heal
- Assistance with a stent, which may be placed in the esophagus to help with swallowing
- Social work support to help navigate homecare, out-of-town housing, emotional support, caretaker needs, health insurance, transportation—or any other concerns you and your family might have
- Pain management services to assist you with pain management and medication
Surgery and Treatment for Diseases of the Esophagus
Johns Hopkins surgeon Dr. Richard Battafarano discusses surgery treatment options for esophageal cancer, including new advances in minimally invasive surgical technology.