Collagenous and Lymphocytic Colitis
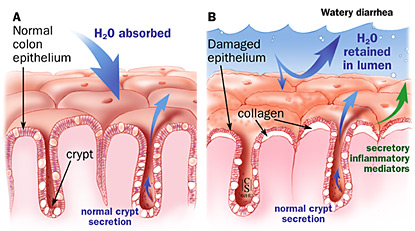
Collagenous and lymphocytic colitis are forms of microscopic colitis that affect the large intestine. The term microscopic colitis is used to describe chronic, watery diarrhea in patients with only microscopic evidence of inflammation.
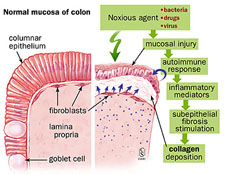
Collagenous and Lymphocytic Colitis Symptoms
The main symptom of collagenous colitis and lymphocytic colitis is chronic, watery diarrhea, as often as five to 10 watery bowel movements per day. More than half of patients cannot pinpoint when their symptoms began.
The diarrhea is usually accompanied by cramps and abdominal pain. These episodes rarely occur at night. Patients are commonly given an incorrect diagnosis of irritable bowel syndrome. One key difference is that patients with collagenous/lymphocytic colitis tend to be older and do not have a history of alternating constipation and diarrhea.
Collagenous and Lymphocytic Colitis Diagnosis
A diagnosis of collagenous/lymphocytic colitis begins with a comprehensive physical exam during which you describe your symptoms and medical history. Other diagnostic procedures include:
Laboratory Tests
Routine blood tests will be ordered to look for any abnormalities. Your doctor may also want to collect a stool sample for analysis.
Endoscopic Diagnosis
The standard diagnostic procedure for collagenous/lymphocytic colitis is a lower endoscopy to examine the lower gastrointestinal tract. The endoscope or colonoscope is flexible and able to accommodate bends in the colon. A colonoscopy allows your doctor to see the largest area, including anus, rectum and colon.
Preparing for a colonoscopy includes:
-
Fasting for eight hours prior to the procedure.
-
Avoiding aspirin for seven days prior to the procedure if a biopsy (removing some tissue for analysis) will be performed. This will minimize the risk of bleeding.
-
Cleaning your colon using a bowel preparation. Your doctor will give you more details before your procedure.
What to expect during a colonoscopy:
-
You receive a sedative and are placed on your left side.
-
The colonoscope is inserted into the rectum and advances through your colon.
-
The colonoscope transmits images to a video monitor.
-
Your doctor examines your gastrointestinal tract and performs a biopsy if necessary.





