Featured Articles
-
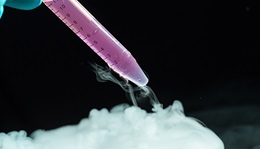 Fertility ProceduresSperm Banking
Fertility ProceduresSperm Banking -
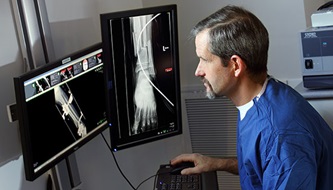
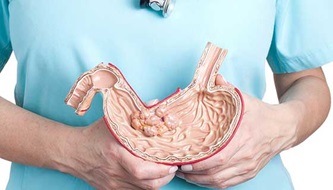
 Stomach cancerHow Endoscopy Detects Stomach Cancer
Stomach cancerHow Endoscopy Detects Stomach Cancer -
 Spine SurgerySpinal Cord Stimulator Removal: Q&A with a Neurosurgeon
Spine SurgerySpinal Cord Stimulator Removal: Q&A with a Neurosurgeon -
 Peripheral Nerve InjuriesNerve Transfer
Peripheral Nerve InjuriesNerve Transfer -
 Food and NutritionFODMAP Diet: What You Need to Know
Food and NutritionFODMAP Diet: What You Need to Know -
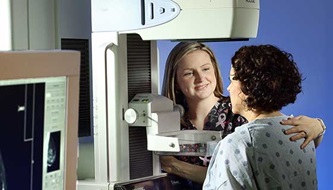
 Diagnosis and ScreeningBreast Biopsy: What You Need to Know
Diagnosis and ScreeningBreast Biopsy: What You Need to Know
Popular Treatments, Tests and Therapies
- Upper GI Endoscopy
- Cholecystectomy
- Colonoscopy
- Radical Prostatectomy
- Colostomy
- Fetal Ultrasound
- Appendectomy
- Cervical Biopsy
- Breast Reconstruction
- Craniotomy
- Scar Revision
- Computed Tomography (CT or CAT) Scan of the Brain
- Electroencephalogram (EEG)
- X-Rays
- Robotic Prostatectomy
- Breast Augmentation
- Pacemaker Insertion
- Knee Replacement Surgery Procedure
- Heart Valve Repair or Replacement Surgery
Know Your Options for Breast Reconstruction
Most women treated for breast cancer are eligible for breast reconstruction—learn about your many options.
Subscribe to Your Health E-Newsletter
Looking for smart, simple tips to help keep you healthy? Your Health is a free, monthly e-newsletter from Johns Hopkins Medicine.
Treatments, Tests and Therapies
- Adrenal Gland Procedures
- Aortic Valve Treatment
- Arrhythmia Treatment
- Back and Spine Surgery
- Biopsies
- Blood Clot Treatment
- Brain Aneurysm Treatment
- Brain Tumor Treatment
- Cardiovascular Aneurysm Treatment
- Cardiovascular Surgery
- Colon Surgery
- Coronary Artery Disease Treatment
- Diagnosis and Screening for Cardiovascular Conditions
- Diagnosis and Screening for Gastric Conditions
- Diagnosis and Screening for Gynecologic Conditions
- Diagnosis and Screening for Orthopaedic Conditions
- Diagnosis and Screening of Urologic Conditions
- Fertility Procedures
- Foot and Ankle Surgery
- Gastric Surgery
- Gynecology Surgery
- Hip Surgery
- Imaging
- Kidney Procedures
- Knee Surgery
- Diagnosis and Screening for Neurological Conditions
- Obesity Treatment Procedures
- Organ Donation and Transplant
- Overview of the PM&R Treatment Team
- Pain Management Procedures
- Pediatric Cardiovascular Procedures
- Pediatric Gastric Procedures
- Pediatric Orthopaedic Procedures
- Pediatric Urology Procedures
- Pericardial Effusion Treatment
- Pregnancy Labor and Delivery
- Prostate Procedures
- Routine Screenings
- Shoulder Surgery
- Sleep Study
- Stroke Treatment