After a patient is triaged from the emergency department, he or she take one of two pathways of care. The sickest and most seriously injured patients are seen first, while other patients may wait longer to be examined by a physician or a physician’s assistant. When they are examined, the provider may look inside the patient’s eyes, ears and throat, or listen to their heart and breathing sounds. After the patient is assessed, the provider may order labs, imaging or medications to ease pain. What if this were all done virtually, with no physician in the room?
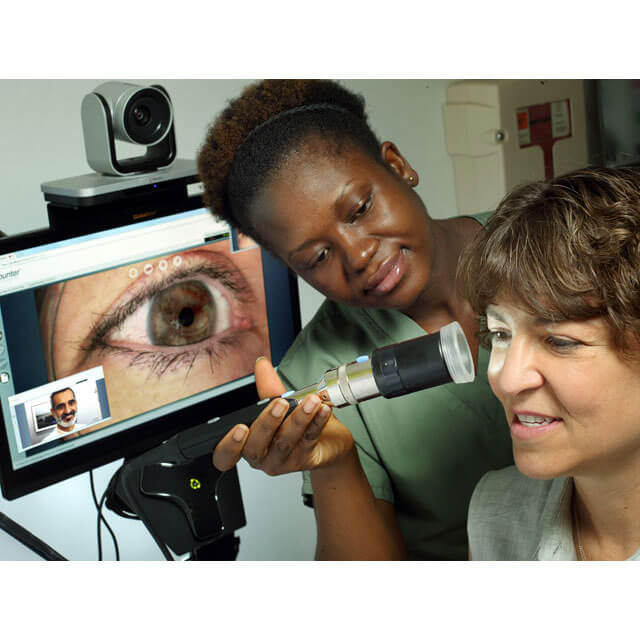
A project that began in January 2017 is doing just that: using telemedicine to screen patients in the emergency departments at The Johns Hopkins Hospital, Howard County General Hospital and Johns Hopkins Bayview Medical Center. Through the use of Epic, the electronic medical records system, the provider views three dashboards, one for each location. With the help of a certified nursing assistant, who facilitates the medical screening, the provider performs the exam with the help of a custom-designed telemedicine cart. The cart allows the physician to see the patient using a remote-controlled camera and to examine that patient using a hand-held camera, and an electronic stethoscope and otoscope. Like FaceTime on an iPhone, a screen allows for real-time conversation between the provider and the patient. Epic stores the patient’s histories and other information gathered during the exam.
Over 4,300 patients have been telescreened by the project, the brainchild of Junaid Razzak, director of telemedicine, and Gai Cole, assistant administrator for the Johns Hopkins Hospital Emergency Department. Cole says the program could potentially be used other times. “If we had a situation where there’s a surge of patients, we can activate a remote provider who is off-shift to help.”
A patient can turn down the option to be telescreened, as all patients have to consent. Fewer than 10 percent of patients opt to see an in-person provider.
After every encounter, feedback is collected on the experience from patients and the provider, and comments have been mostly positive, he says. Some patient comments include: “Wow, this is so innovative and cool. It’s like I’m Skyping with my doctor,” and “It’s so cool I can see what the doctor sees on the cart. I like being a part of my own care.”
And the physicians are commenting on the value, as well: “Technology works well. I am able to screen effectively,” and “Definitely helps the provider in the morning get caught up in most circumstances.”
Cole says his team members are already seeing the benefits virtual exams have on wait times and access to care, and telescreening is just the emergency department’s first entry in the telemedicine world. The team is exploring models of teaching using telemedicine and projects for some international Johns Hopkins sites. They are also looking at other venues outside of the emergency department.
“We would also like to use this technology in the very near future to assess patients who might otherwise come to the emergency department for assessment,” says Cole. “Nursing homes, for example, present an opportunity to leverage this technology to prevent avoidable visits. If you can turn on a telemedicine system, you can have a meaningful consult right there.”