In five short years, the Department of Plastic and Reconstructive Surgery has grown from a modest-sized division to an independent, flourishing department that is second to none for scientific discovery and clinical advances. It has quickly developed a global reputation for its cutting-edge techniques, groundbreaking research and surgeons who are deeply driven to deliver the best possible care to their patients. Highlights of those five years include:
A 2010 gift from Milton Edgerton, the first full-time plastic surgery chief at Johns Hopkins, and the blue moon fund established the Milton T. Edgerton, M.D., Professorship and Directorship of Plastic and Reconstructive Surgery, held since then by department director W.P. Andrew Lee.
A comprehensive research laboratory has been established conducting scientific investigation in transplant immunology, regenerative medicine, cutaneous cancer biology and nerve research and stem cell biology. Laboratory personnel now include three full-time research faculty members and about 20 pre- and postdoctoral fellows and technicians. Departmental sponsored research funding has increased some 20-fold on an annual basis (see graph). This research support comes from a variety of government, foundation, industry and institutional sources. Department of Defense funds make up approximately 80 percent of the total, with NIH, multiple foundation and industry grants making up the balance.
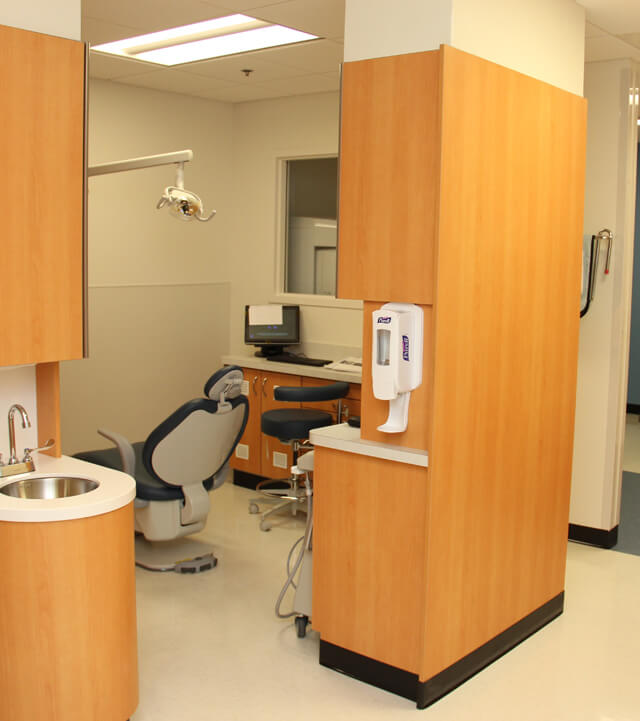 In spring 2015, the department opened a state-of-the-art craniofacial center and high-tech dental lab to support the pediatric cleft and craniofacial program. The center will be capable of full digital imaging, planning and support of three-dimensional modeling.
In spring 2015, the department opened a state-of-the-art craniofacial center and high-tech dental lab to support the pediatric cleft and craniofacial program. The center will be capable of full digital imaging, planning and support of three-dimensional modeling.
Over the past five years, the department has added one full professor, three associate professors and 10 assistant professors, including the department’s first faculty member at Johns Hopkins All Children’s Hospital in St. Petersburg, Florida.
 In 2014, the VCA Journal was launched with Gerald Brandacher, scientific director of the reconstructive transplantation program, serving as editor-in-chief. The publication is the official journal of The American Society for Reconstructive Transplantation and chronicles advances in the field of vascularized composite allotransplantation.
In 2014, the VCA Journal was launched with Gerald Brandacher, scientific director of the reconstructive transplantation program, serving as editor-in-chief. The publication is the official journal of The American Society for Reconstructive Transplantation and chronicles advances in the field of vascularized composite allotransplantation.
Department faculty members Chad Gordon, Damon Cooney and Amir Dorafshar have been named recipients of the prestigious American Association of Plastic Surgeons Academic Scholarship Awards for three years in a row. The annual awards recognize young investigators deemed most likely to advance knowledge in their field. Award funds help them establish and support their own research laboratories.
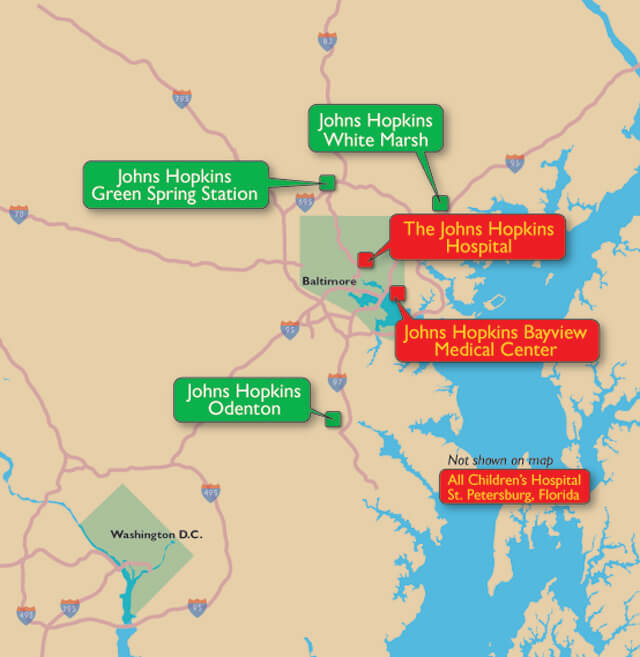 The department has an expanded presence in clinical activities including Johns Hopkins Bayview Medical Center, Johns Hopkins Green Spring Station, Johns Hopkins White Marsh, Greater Baltimore Medical Center, Johns Hopkins Odenton and All Children’s Hospital (St. Petersburg, Florida), in addition to its home base of The Johns Hopkins Hospital.
The department has an expanded presence in clinical activities including Johns Hopkins Bayview Medical Center, Johns Hopkins Green Spring Station, Johns Hopkins White Marsh, Greater Baltimore Medical Center, Johns Hopkins Odenton and All Children’s Hospital (St. Petersburg, Florida), in addition to its home base of The Johns Hopkins Hospital.
The past five years have seen the launch of several new department programs. These include Hand/Arm Transplant, Face Transplant, Non-Breast Oncologic Reconstruction, Lymphedema and Penile Transplant. The penile transplant program was established after years of research and development of novel surgical techniques to better perfuse the graft and enhance nerve regeneration. It aims to restore genitourinary function in servicemen and civilians who have suffered devastating injuries to the pelvic region.
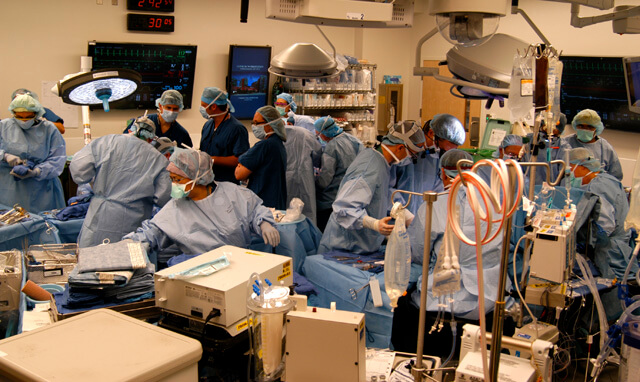 The reconstructive transplant team performed the nation’s most extensive and complicated bilateral arm transplant in 2012 in a quadruple amputee soldier. That success laid the foundation for another above-elbow transplant, in 2015. The department’s hand transplant surgeons have performed three of the four above-elbow transplants in the U.S. to date.
The reconstructive transplant team performed the nation’s most extensive and complicated bilateral arm transplant in 2012 in a quadruple amputee soldier. That success laid the foundation for another above-elbow transplant, in 2015. The department’s hand transplant surgeons have performed three of the four above-elbow transplants in the U.S. to date.
 The ranks of residents in the combined Johns Hopkins/University of Maryland program have grown from 18 in 2010 to 30 in 2016 and will continue to grow. The shift from divisional to departmental status led to an expansion of services, programs and faculty, which provided more surgeries and clinical learning opportunities for residents. New postgraduate fellowships have been added in hand surgery and microsurgery to the existing craniofacial and burn programs, training a total of six fellows every year.
The ranks of residents in the combined Johns Hopkins/University of Maryland program have grown from 18 in 2010 to 30 in 2016 and will continue to grow. The shift from divisional to departmental status led to an expansion of services, programs and faculty, which provided more surgeries and clinical learning opportunities for residents. New postgraduate fellowships have been added in hand surgery and microsurgery to the existing craniofacial and burn programs, training a total of six fellows every year.
