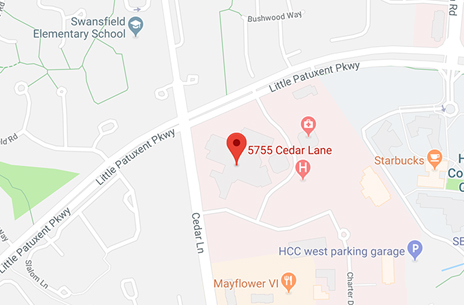
Johns Hopkins Howard County Medical Center combines the convenience of a full range of hospital and wellness services, more than 1000 affiliated doctors in nearly 100 clinical specialties, award winning clinical excellence and membership in Johns Hopkins Medicine, one of the country’s premier academic medical systems.