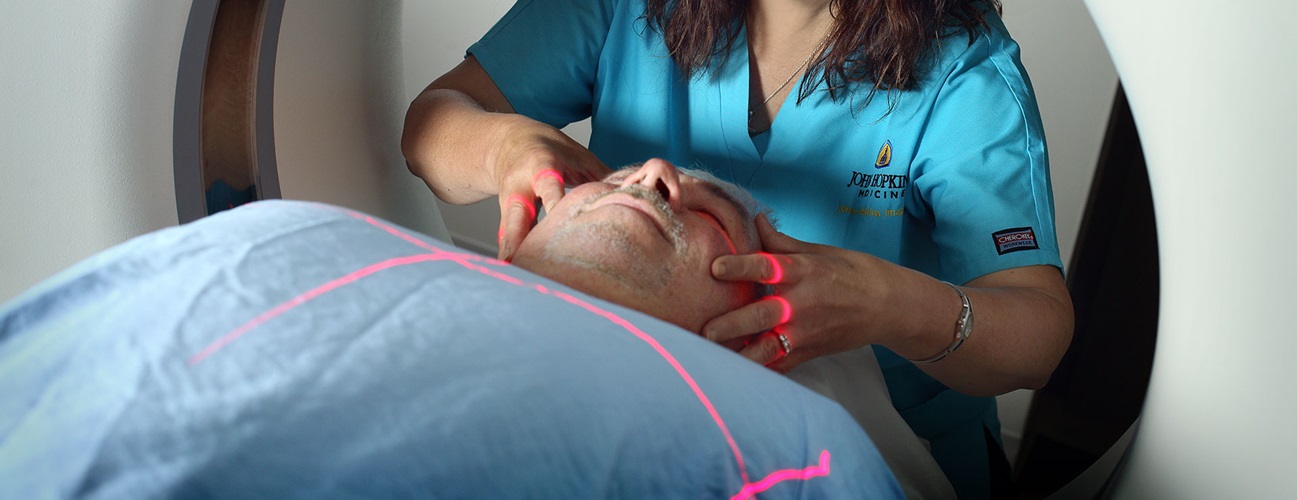
Positron Emission Tomography (PET)
What is positron emission tomography (PET)?
Positron emission tomography (PET) is a type of nuclear medicine procedure that measures metabolic activity of the cells of body tissues. PET is actually a combination of nuclear medicine and biochemical analysis. Used mostly in patients with brain or heart conditions and cancer, PET helps to visualize the biochemical changes taking place in the body, such as the metabolism (the process by which cells change food into energy after food is digested and absorbed into the blood) of the heart muscle.
PET differs from other nuclear medicine examinations in that PET detects metabolism within body tissues, whereas other types of nuclear medicine examinations detect the amount of a radioactive substance collected in body tissue in a certain location to examine the tissue's function.
Since PET is a type of nuclear medicine procedure, this means that a tiny amount of a radioactive substance, called a radiopharmaceutical (radionuclide or radioactive tracer), is used during the procedure to assist in the examination of the tissue under study. Specifically, PET studies evaluate the metabolism of a particular organ or tissue, so that information about the physiology (functionality) and anatomy (structure) of the organ or tissue is evaluated, as well as its biochemical properties. Thus, PET may detect biochemical changes in an organ or tissue that can identify the onset of a disease process before anatomical changes related to the disease can be seen with other imaging processes such as computed tomography (CT) or magnetic resonance imaging (MRI).
PET is most often used by oncologists (doctors specializing in cancer treatment), neurologists and neurosurgeons (doctors specializing in treatment and surgery of the brain and nervous system), and cardiologists (doctors specializing in the treatment of the heart). However, as advances in PET technologies continue, this procedure is beginning to be used more widely in other areas.
PET may also be used in conjunction with other diagnostic tests, such as computed tomography (CT) or magnetic resonance imaging (MRI) to provide more definitive information about malignant (cancerous) tumors and other lesions. Newer technology combines PET and CT into one scanner, known as PET/CT. PET/CT shows particular promise in the diagnosis and treatment of lung cancer, evaluating epilepsy, Alzheimer's disease and coronary artery disease.
Originally, PET procedures were performed in dedicated PET centers, because the equipment to make the radiopharmaceuticals, including a cyclotron and a radiochemistry lab, had to be available, in addition to the PET scanner. Now, the radiopharmaceuticals are produced in many areas and are sent to PET centers, so that only the scanner is required to perform a PET scan.
Further increasing the availability of PET imaging is a technology called gamma camera systems (devices used to scan patients who have been injected with small amounts of radionuclides and currently in use with other nuclear medicine procedures). These systems have been adapted for use in PET scan procedures. The gamma camera system can complete a scan more quickly, and at less cost, than a traditional PET scan.
How does PET work?
PET works by using a scanning device (a machine with a large hole at its center) to detect photons (subatomic particles) emitted by a radionuclide in the organ or tissue being examined.
The radionuclides used in PET scans are made by attaching a radioactive atom to chemical substances that are used naturally by the particular organ or tissue during its metabolic process. For example, in PET scans of the brain, a radioactive atom is applied to glucose (blood sugar) to create a radionuclide called fluorodeoxyglucose (FDG), because the brain uses glucose for its metabolism. FDG is widely used in PET scanning.
Other substances may be used for PET scanning, depending on the purpose of the scan. If blood flow and perfusion of an organ or tissue is of interest, the radionuclide may be a type of radioactive oxygen, carbon, nitrogen, or gallium.
The radionuclide is administered into a vein through an intravenous (IV) line. Next, the PET scanner slowly moves over the part of the body being examined. Positrons are emitted by the breakdown of the radionuclide. Gamma rays called annihilation photons are created when positrons collide with electrons near the decay event. The scanner then detects the annihilation photons, which arrive at the detectors in coincidence at 180 degrees apart from one another. A computer analyzes those gamma rays and uses the information to create an image map of the organ or tissue being studied. The amount of the radionuclide collected in the tissue affects how brightly the tissue appears on the image, and indicates the level of organ or tissue function.

Why is PET performed?
In general, PET scans may be used to evaluate organs and/or tissues for the presence of disease or other conditions. PET may also be used to evaluate the function of organs, such as the heart or brain. The most common use of PET is in the detection of cancer and the evaluation of cancer treatment.
More specific reasons for PET scans include, but are not limited to, the following:
-
To diagnose dementias (conditions that involve deterioration of mental function), such as Alzheimer's disease, as well as other neurological conditions such as:
-
Parkinson's disease. A progressive disease of the nervous system in which a fine tremor, muscle weakness, and a peculiar type of gait are seen.
-
Huntington's disease. A hereditary disease of the nervous system which causes increasing dementia, bizarre involuntary movements, and abnormal posture.
-
Epilepsy. A brain disorder involving recurrent seizures.
-
Cerebrovascular accident (stroke)
-
-
To locate the specific surgical site prior to surgical procedures of the brain
-
To evaluate the brain after trauma to detect hematoma (blood clot), bleeding, and/or perfusion (blood and oxygen flow) of the brain tissue
-
To detect the spread of cancer to other parts of the body from the original cancer site
-
To evaluate the effectiveness of cancer treatment
-
To evaluate the perfusion (blood flow) to the myocardium (heart muscle) as an aid in determining the usefulness of a therapeutic procedure to improve blood flow to the myocardium
-
To further identify lung lesions or masses detected on chest X-ray and/or chest CT
-
To assist in the management and treatment of lung cancer by staging lesions and following the progress of lesions after treatment
-
To detect recurrence of tumors earlier than with other diagnostic modalities
Find an Imaging Location

How is PET performed?
PET scans can be done on an outpatient basis. It is also possible that some hospital inpatients may undergo a PET examination for certain conditions.
Although each facility may have specific protocols in place, generally, a PET scan procedure follows this process:
-
The patient will be asked to remove any clothing, jewelry, or other objects that may interfere with the scan.
-
If asked to remove clothing, the patient will be given a gown to wear.
-
The patient will be asked to empty his or her bladder prior to the start of the procedure.
-
One or 2 IV lines will be started in the hand or arm for injection of the radionuclide.
-
Certain types of scans of the abdomen or pelvis may require that a urinary catheter be inserted into the bladder to drain urine during the procedure.
-
In some cases, an initial scan may be performed prior to the injection of the radionuclide, depending on the type of study being done. The patient will be positioned on a padded table inside the scanner.
-
The radionuclide will be injected into the IV. The radionuclide will be allowed to concentrate in the organ or tissue for about 30 to 60 minutes. The patient will remain in the facility during this time. The patient will not be hazardous to other people, as the radionuclide emits less radiation than a standard X-ray.
-
After the radionuclide has been absorbed for the appropriate length of time, the scan will begin. The scanner will move slowly over the body part being studied.
-
When the scan has been completed, the IV line will be removed. If a urinary catheter has been inserted, it will be removed.