Anesthesia
What is anesthesia?
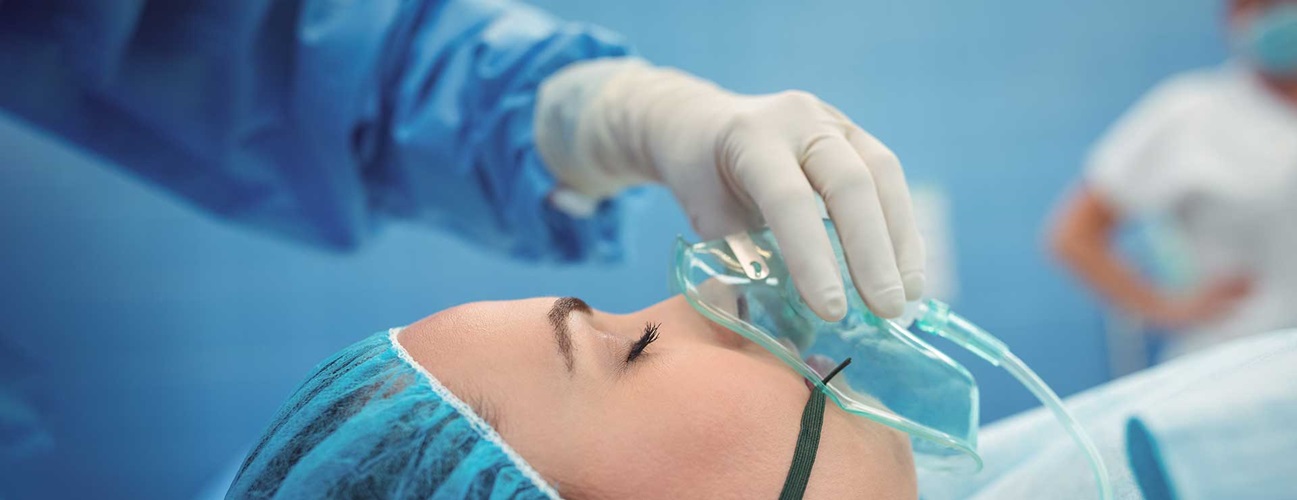
During surgery, you'll be given anesthesia. This is medicine to relieve pain and feeling during surgery. An anesthesiologist or certified nurse anesthetist gives the type and dosage of anesthesia. This is a healthcare provider with extra training in using this medicine safely. Before surgery, you'll meet with this healthcare provider. They will review your condition and health history to plan the right anesthetic for you.
Types of anesthesia
There are different types of anesthesia. The type you get will depend on the type of surgery and your overall health. You may also be given a sedative. This is medicine to make you sleepy. Pain medicine may also be used. The different types of anesthesia include:
Local anesthesia
Local anesthesia is given for a short time to stop pain in one part of the body. You stay awake. For minor surgery, a local anesthetic can be injected into the area. Or it may be absorbed into the skin. If a large area needs to be numbed, or if a local anesthetic injection won't work well enough, another type of anesthesia may be used.
Regional anesthesia
Regional anesthesia is used to numb only the part of the body that will have the surgery. First, a local anesthetic is injected into the area of nerves that provide feeling to that part of the body. Then, a regional anesthesia is used. There are two forms of regional anesthetics:
-
Spinal anesthetic. This is used for lower abdominal, pelvic, rectal, or lower extremity surgery. A single dose of the anesthetic is injected into the area around the spinal cord. The injection is done in the lower back. It causes numbness in the lower body. This type of anesthesia is most often used for surgery of the legs or hips.
-
Epidural anesthetic. This is similar to spinal anesthetic. It's often used for surgery of the lower limbs or during labor and childbirth. This type of medicine is given ongoing through a thin tube (catheter). The catheter is placed into the space around the spinal cord in the lower back. It causes numbness in the lower body. An epidural may also be used for chest or abdominal surgery. In this case, the medicine is injected at a higher place in the back. This then numbs both the chest and abdominal areas.
General anesthesia
General anesthesia is medicine that is used to put you in a state like deep sleep during surgery. The medicine may be inhaled through a breathing mask or tube. Or it may be given through an IV (intravenous) line. A breathing tube may be inserted into your windpipe. This is to help you breathe during surgery. Once the surgery is done, the medicine is stopped. You're taken to a recovery area and watched closely.
What does an anesthesiologist do?
These healthcare providers are trained to manage anesthesia during surgery. They also manage and treat changes in your breathing, heart rate, and blood pressure during surgery. They also diagnose and treat any medical problems that might happen during and right after surgery.
If you have a condition, such as diabetes, asthma, heart problems, or arthritis, your anesthesia care provider will have been told. They will be prepared to manage these conditions during and right after your surgery as needed. Anesthesia care providers aren't just trained to handle medical issues related to the surgery. They also handle any chronic conditions that may need attention during the surgery.
Because anesthesia and surgery affect every system in the body, the anesthesia care provider will interview you before surgery. Sometimes this is done in person. In other cases, they will do the interview over the phone. During this interview, the anesthesia care provider will review your health history. They will also tell you about what to expect during your surgery and discuss anesthetic choices with you. This is also the time to discuss which medicines should be stopped, and which can continue before surgery. The anesthesia care provider will also let you know when you'll need to stop eating before the surgery.
What to tell your anesthesia care provider
Before surgery, this provider will check your health. They will select an anesthetic that is safe for your health. It's vital that the provider knows as much about your health as possible. This includes your full health history, lifestyle, and medicines. Make sure you have told the healthcare team about all medicines, vitamins, and herbal supplements you take. Tell the provider and the healthcare team if you:
-
Have had a reaction to anesthesia in the past. If you've ever had a bad reaction to anesthesia, you need to be able to describe what the reaction was. Give as much detail as possible. Did you have nausea when you woke up? Did it take a long time for you to wake up?
-
Are taking any herbal supplements. Some common herbal products may cause changes in heart rate and blood pressure. They may also increase bleeding. Gingko biloba, garlic, ginger, and ginseng may lead to too much blood loss. They do this by preventing blood clots from forming. St. John's wort and kava kava may cause the effects of the anesthetic to last too long. Stop taking all herbal supplements at least 2 to 3 weeks before surgery.
-
Have any allergies. Discuss any known allergies with the anesthesiologist. Some anesthetic drugs trigger cross-allergies, particularly in people who have allergies to eggs and soy products. Report allergies to both foods and drugs.
-
Are taking any medicines. This includes all prescription and over-the-counter medicines. Some medicines that thin the blood, such as aspirin or warfarin, must be stopped for several days or longer before surgery. Other medicines can cause too much bleeding or cause problems with anesthesia.
-
Smoke cigarettes. Cigarette smoking affects the lungs, heart, liver, and blood. This can change the way anesthesia works during surgery. Tell your healthcare providers about your past, recent, and current smoking. Surgery can be a good time to quit smoking. Most hospitals are smoke-free. Healthcare providers will be there to give you support. You'll heal and recover faster. Skin and bones heal more slowly if you smoke. Quitting smoking before surgery also lessens the risk of lung problems after surgery, such as pneumonia. Quitting smoking also reduces your risk of heart disease, lung disease, and cancer.
-
Drink alcohol. Alcohol can also affect your heart, liver, and blood. It can also change the way anesthesia works during surgery. Tell your healthcare providers about your history of alcohol use before surgery.
-
Use of street drugs. This includes marijuana, cocaine, amphetamines, and others. This is because these drugs can affect healing and responses to anesthesia. You may not want to talk about using these drugs. But keep in mind that this is private information between you and your providers. They need to know this information in order to give you the right anesthesia. Tell your healthcare team about your past, recent, and current use of drugs.
What happens during surgery?
The anesthesia care provider will meet with you right before your surgery to review your entire health history, as well as the results of any medical tests previously done. By this time, they will have a clear understanding of your anesthetic needs.
The anesthesia care provider will give you the anesthesia medicines during the surgery. And they will also monitor your health very closely. This is one of the most important roles this provider has during surgery. They will closely watch for the slightest changes in a wide range of your body functions, such as heart rate and rhythm, blood pressure, body temperature, oxygen levels, and breathing. This gives a lot of information about your well-being. They will also manage fluid and blood replacement, when needed.
What happens after surgery?
After surgery, you'll be moved to a recovery area. Your healthcare team will closely watch your heart rate, blood pressure, and other vital signs. When the anesthesia wears off, you'll go to your hospital room or be allowed to go home.