Staph Infection
What is a staphylococcal infection?
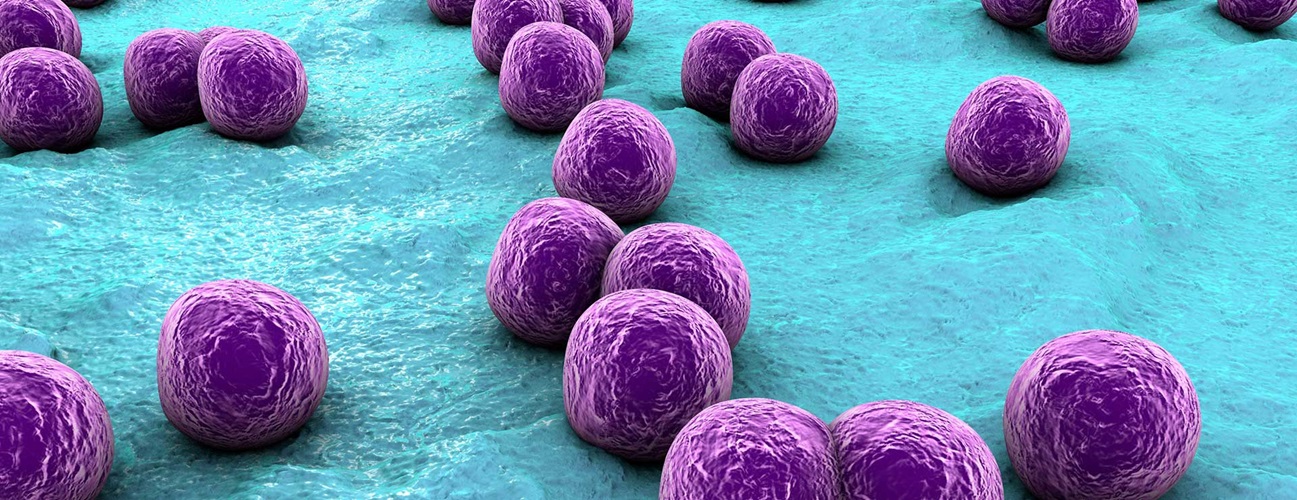
Staphylococcus aureus, or “staph,” are common bacteria that normally live on the skin. The bacteria also live harmlessly in the nasal passages of roughly 30 percent of the U.S. population. Staph can cause infection when they enter the skin through a cut or sore. Infection can also occur when the bacteria move inside of the body through a catheter or breathing tube.
Staphylococcus aureus, or S. epidermidis, can cause staphylococcal meningitis, an infection of the membranes covering the brain and spinal cord caused by; it usually develops as a complication of a surgical procedure or a blood-borne infection.
Diagnosis
Depending on the extent and severity of your symptoms, your doctor may recommend the following tests:
-
A skin biopsy and culture from the infected site
-
Culture of the drainage (fluid) from the infection, to see which organism grows in it
-
Blood culture
-
Sputum culture through coughing or bronchoscopy if pneumonia is present or suspected
-
Urine culture if a urinary tract infection is present or suspected
Treatment
Treatment depends on the type of staph infection. Some require intravenous antibiotics. For a local Methicillin-resistant Staphylococcus aureus (MRSA) skin infection, draining the abscess at the doctor's office is usually the only treatment needed. Few antibiotics are available to treat more serious MRSA infections. These include vancomycin (Vancocin, Vancoled), trimethoprim-sulfamethoxazole (Bactrim, Bactrim DS, Septra, Septra DS) and linezolid (Zyvox).
Note: It is critically important to finish all doses of antibiotics you have been given, even if you feel better before the final dose. Unfinished doses can lead to development of drug resistance in the bacteria.