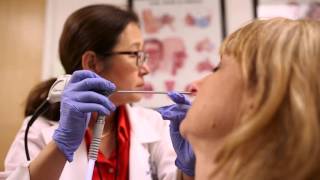
Nasal Polyps
Reviewed By:
Nasal polyps are noncancerous growths of the tissues that line the nose and sinuses. These growths are often shaped like teardrops and form in groups.
Symptoms
Common symptoms include:
- Difficulty breathing through your nose
- Decreased sense of smell
- Decreased sense of taste
- Postnasal drip
- Runny nose
- Headache
- Cough
- Facial pain or pain in upper teeth
- Pressure around sinuses
- Itching around the eyes
- Snoring
Causes
The development of nasal polyps is associated with chronic rhinosinusitis, which is inflammation of the nasal passages and sinuses lasting 12 weeks or more. The cause of nasal polyps is not fully understood because of the complexity of the condition. But research suggests those affected may have an abnormal immune response and different chemical markers in their mucus membrane (which lines the sinuses and nasal cavity), compared to those who do not develop nasal polyps. These chemical markers act like signs telling the body what it is and how to react. This is an active area of study that is in much need of investigation.
Diagnosis
Nasal polyps should be diagnosed by your doctor, who will use a nasal endoscope, which is a small thin telescope with a camera on the end, to see inside your nose. In some cases your doctor may take a small sample, called a biopsy, of the growth. CT or MRI scans of the sinuses can also show findings that suggest presence of nasal polyps.
Treatment
Medication: The first course of treatment for nasal polyps is often a nasal corticosteroid spray prescribed by your doctor. For many people, this can shrink or remove nasal polyps. Oral corticosteroids may also be used.
For many with nasal polyps, they return if the irritation, allergy, infection or inflammation continues. Antihistamines and decongestants may help with allergy symptoms that may lead to the development of nasal polyps, but these medications do not directly address the nasal polyps themselves.
Surgery: If the nasal polyp isn’t removed or shrunk by medication, then endoscopic surgery may be required to remove the polyps. Your surgeon will remove the polyp, which is preventing the flow of sinus and nasal fluids from properly draining and ventilating your sinus and nasal passages. This surgery is most often completed as an outpatient procedure.
Prognosis and Prevention
Following surgery, it is important that proper care is taken of the nasal area. Nasal polyps, if not treated correctly, will likely return.
The following strategies are used to prevent nasal polyps from returning:
Continue using a corticosteroid spray. A corticosteroid spray will help reduce inflammation following surgery. Your doctor will be able to prescribe these and other specific treatments tailored to your needs.
Use a humidifier. When the air in your environment becomes dry, especially during winter and in arid climates, a humidifier will help moisten your nasal passages. This improves the flow of mucus in your sinuses, preventing blockage and inflammation that can lead to nasal polyps returning.
Use a nasal spray or rinse. Nasal sprays and rinses help moisten your nasal passages and prevent inflammation. Washing the sinus and nasal cavities with sterile saline solution is also important to heal properly.
Avoid nasal irritants. Dust, debris, smoking and common allergens can cause inflammation in the nasal passages and sinuses. Avoid known nasal irritants as best as you can.
Manage allergies and asthma. Follow your doctor’s treatment plan for managing asthma and allergies. If you symptoms persist, talk to your doctor about changing your individualized plan.
Sinus Surgery | Nici's Story
After two unsuccessful sinus surgeries to treat nasal polyps that she had for 20 years, Virginia resident Nici found help from Johns Hopkins sinus surgeon Jean Kim. Learn how Kim approached treating Nici’s condition and how Nici’s quality of life has improved.