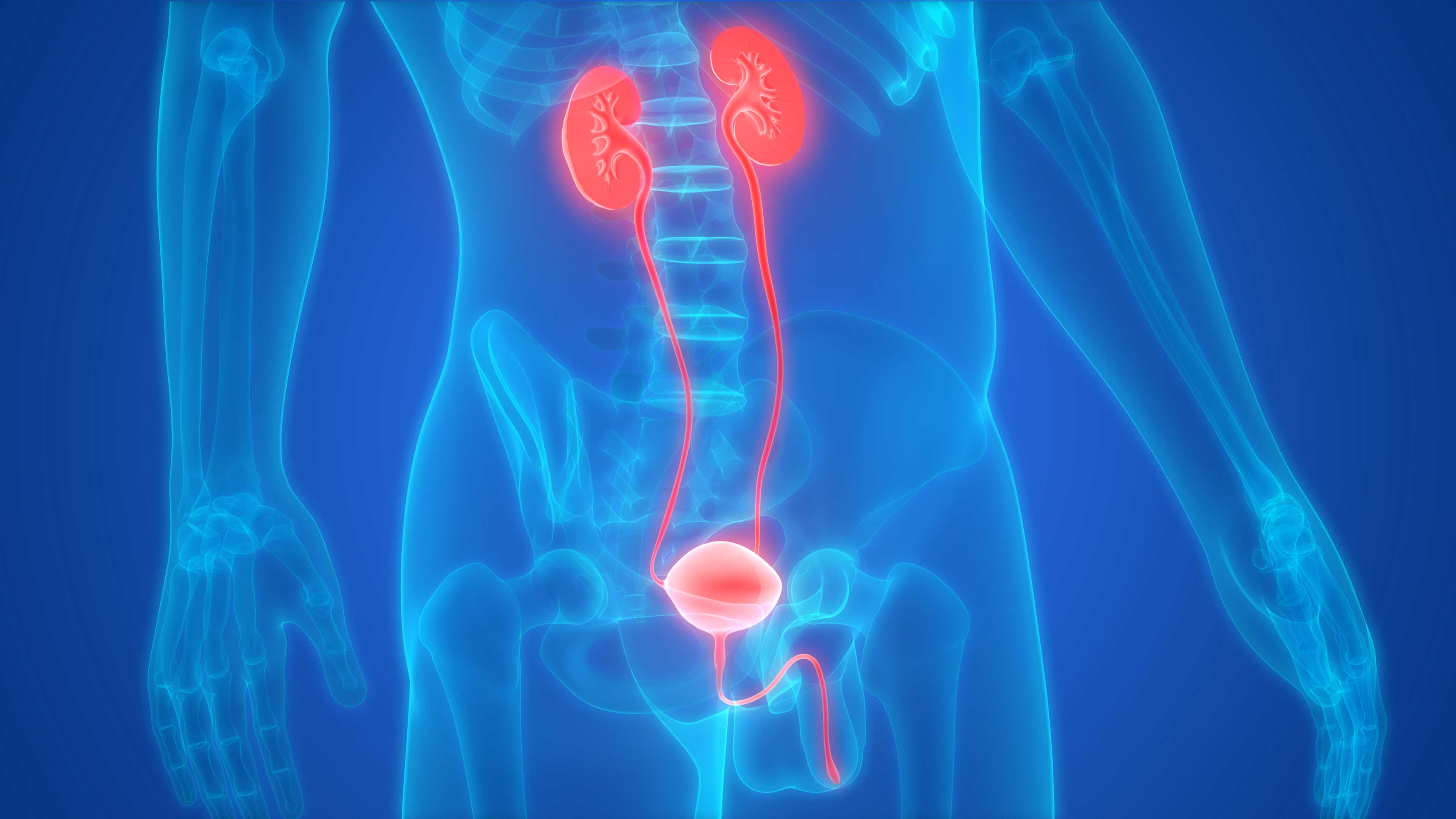
Bladder Cancer Treatment
Over 75 percent of bladder cancers remain confined to the lining of the bladder and do not invade the bladder wall. These are called nonmuscle-invasive bladder cancer, or superficial bladder cancer, and when managed well, they are associated with excellent prognoses.
Muscle-invasive bladder cancer, or advanced bladder cancer, is cancer that has invaded the bladder wall or spread outside of the bladder. These cancers require more aggressive clinical management.
Bladder cancer treatment options vary depending on whether the cancer is nonmuscle-invasive or muscle-invasive, and specific treatments are determined based on the stage and grade of the tumor(s).
Treatments for Nonmuscle-Invasive (Superficial) Bladder Cancer
Cystoscopy with Cautery Destruction of the Bladder Tumor
Cystoscopy is an outpatient procedure during which a thin, lighted tube with a camera is passed through the urethra into the bladder, allowing your doctor to see the inside of the bladder.
Most modern cystoscopes are also equipped with channels that permit small instruments to be passed into the bladder. During a cystoscopy, your doctor may use these instruments to remove tissue, stop bleeding with a special electrical device called an electrocautery or even perform laser treatment. If the bladder cancer tumor is small enough, this cautery may be used to remove the cancer.
Transurethral Resection of the Bladder Cancer Tumor
This is when the tumor is removed from the urinary tract through the urethra using an electrical force. Transurethral resection (TUR) is an endoscopic or scope procedure that does not involve making an incision in the body.
Drug therapy after TUR is commonly prescribed for patients with large, multiple or high-grade tumors.
Intravesical Drug Therapy (Chemotherapy and Immunotherapy)
Intravesical drug therapy involves placing medicines directly into the bladder via a urethral catheter to lower the recurrence rates of bladder tumors. It is usually used for multiple carcinomas in situ that cover a large area (5 centimeters-plus), or for high-grade or high-stage tumors.
Commonly used intravesical drugs are:
- Mitomycin C is a chemotherapy drug that kills the normal DNA function in cancer cells and is easily absorbed into the bloodstream through the bladder's lining.
- Bacille Calmette–Guerin (BCG) is an immunotherapy drug that makes the body’s immune system respond to the BCG drug in the lining of the bladder, forcing the immune system to help fight off the cancer. About 50 to 68 percent of patients with nonmuscle-invasive bladder cancer have a very good response to BCG.
Bladder Cancer | Q&A
Understand the basics of bladder cancer, from risk factors and diagnosis to the various treatment and urinary diversion options available. Armine Smith, M.D., a surgeon at the Johns Hopkins Greenberg Bladder Cancer Institute, tells you what you need to know.
Treatments for Muscle-Invasive (Advanced) Bladder Cancer
Cystectomy (Bladder Removal) Surgery
When bladder cancer tumors completely invade the bladder’s muscular wall, the standard of care is to perform bladder removal surgery. Typically, complete removal of the bladder (radical cystectomy) is required.
Partial cystectomy is rare because the requirements are that the tumor is easily accessible and small in size, and that there are no tumors in the rest of the bladder. This approach is usually used only if the cancer has not left its site of origin. Additionally, partial cystectomy may be an alternative option for nonmuscle-invasive bladder cancer if all other treatments fail.
Radiation Therapy
Radiation therapy, used to treat cancer, is a special high-energy X-ray that is more powerful than the X-rays used for imaging studies. Radiation therapy is planned and executed in a way to kill cancer cells or alter their ability to reproduce, while the surrounding healthy cells are minimally affected.
Historically, radiation therapy alone has been used for muscle-invasive bladder cancer, but current treatment usually involves a combined approach of maximal local surgery, radiation and chemotherapy. The role of radiation therapy in this combined approach is to kill the bladder cancer cells in the bladder that are not visible to the surgeon. Chemotherapy is used to enhance the effects of the radiation and kill cells outside the bladder. Local lymph nodes are frequently radiated as part of the therapy to treat the microscopic cancer cells that may be there.
Chemotherapy
Chemotherapy uses chemical agents to interfere with replication and other normal functions of cells, resulting in tumor shrinkage or cancer cell death. The use of two or more chemotherapy drugs together has been found to be more effective than a single drug alone. There are several types of chemotherapy. The most common chemotherapeutic drug used in bladder cancer is cisplatin.
Immunotherapy
Immunotherapy is a cancer treatment approach that uses drugs and vaccines to harness the immune system’s natural ability to fight cancer, in the same way it fights off infections. The approach is still being researched and there is a lot left to learn, but clinical studies have shown that immunotherapy holds a lot of promise in its ability to treat a wide range of malignancies, including some types of bladder cancer.
There are a few FDA-approved immunotherapy drugs available for treating advanced and metastatic bladder cancer that has worsened after chemotherapy. Scientists are also investigating the possibility that combinations of immunotherapy drugs could be more effective than individual drugs.
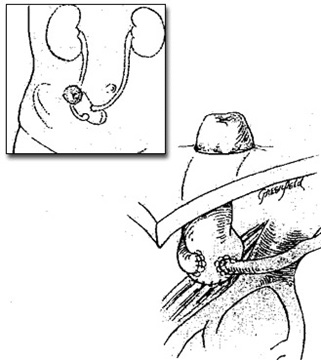
Types of Surgical Reconstruction to Replace the Removed Bladder
Ileal Conduit
This procedure has been routinely performed since the 1950s. The internal pouch that holds the urine is made from a small portion of intestinal tract. One end is closed with sutures, while the other end is attached to skin on the front side of the abdomen. A stoma is the open end of the conduit attached to the skin. An external appliance (ostomy bag) covers the stoma to collect urine. The ureters are implanted into the back of the ileal conduit.
Catheterizable Continent Diversion Pouch
This is a reservoir of bowel with a stoma that is catheterizable for emptying the bladder. The urine is siphoned out of the urinary reservoir with a small catheter every four to six hours. The catheterizable pouch may require surgical repair at some point after surgery due to the wear and tear of frequent catheterization. This type of reconstruction is not performed on patients with a history of bowel disease.
Neobladder
A neobladder is a new bladder made from a section of the patient’s small intestine. This internal, new bladder is connected to the urethra and ureters. After this reconstruction, the patient needs to relearn how to void. Some disadvantages of this type of reconstruction are the possibility of incontinence and scar tissue formation at the connection of the urethra and new bladder.
Minimizing the Impact of Bladder Cancer: Organ Preservation in Male and Female Cystectomy

Learn more about who is a candidate for organ preservation in cystectomy for bladder cancer during this webinar with urologic oncologist Armine Smith.