Capillary Malformation
What are CMs?
Capillary malformation (CM) is a type of vascular anomaly, which is an anomaly or disorder of the vascular system, either in veins or arteries.
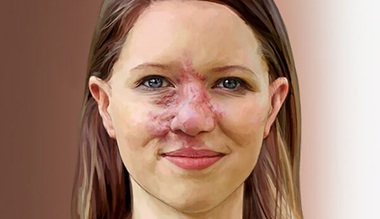
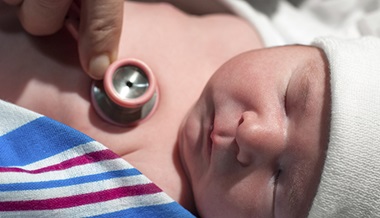
CMs are commonly known as port wine stains. They look like a pink, red or purple patch of skin and occur in 1 in 300 newborns. CMs are present at birth and can occur anywhere on the skin.
It is very rare to develop CMs as an adult. These patches may be light in color at first, but can get darker over time. In adults, CMs can thicken and develop bumps or ‘blebs’ that can sometimes bleed.
CM occurs when skin containing blood vessels has extra blood vessels close to the skin surface.

© Eleanor Bailey
How are CMs diagnosed?
A doctor will diagnose a CM by examining the mark and asking questions about the patient’s history. For simple CMs, other imaging studies are not needed to diagnose them.
When located on the forehead or upper face, CMs can be associated with a condition called Sturge-Weber syndrome. Infants with a CM in this location are at risk for eye and brain problems. They need to have eye exams with an ophthalmologist. They should also be seen by a neurologist, who may order a test called an electroencephalogram (EEG) to look at brain waves, or an MRI.
Nevus simplex are a type of CM that occur as faint pink patches with feathery borders on the eyelids, on the forehead between the eyebrows or around the sides of the nose in newborns. They are commonly called “stork bites” or “angel kisses.” Nevus simplex fade in the first few years of life. When they occur on the nape of the neck they do not disappear, but they are soon covered by hair.
On the body, most commonly on the legs, nevus simplex can sometimes be on top of deeper vascular birthmarks, such as venous malformations, lymphatic malformations or arteriovenous malformations. An MRI or magnetic resonance angiography (MRA) is needed to see the areas below the CM and provide an image of the blood vessels in the vascular birthmark. A CT scan is used to see whether any bone growth has occurred in the area.
Our Approach to Treating Vascular Anomalies
Johns Hopkins Medicine has developed a multidisciplinary Vascular Anomalies Center in order to offer patients individualized treatment. As a leader in diagnosing, researching and treating vascular anomalies and vascular tumors, our team of specialists provide comprehensive treatment and care.
How are CMs treated?
Most CMs cannot be cured, but there are ways to treat and manage this condition.
When CMs occur with other vascular birthmarks beneath the skin, the treatment team often includes interventional radiologists (doctors who can read pictures and scans of your body and offer treatments for the affected blood vessels), general or plastic surgeons, dermatologists, and sometimes hematologists and geneticists.
If the CM affects only the skin, a dermatologist — a doctor who specializes in skin, hair and nails — will manage the treatment with lasers.
Lasers are the most common treatment for CMs. If thickening, bumps or bleeding occur, surgery may be needed. Laser treatment can start in early infancy. Response to laser treatment is often better in younger children compared to adults.
Research is being done to see whether medications can improve the response to laser treatment. There are some reports of a treatment that combines a medicine called sirolimus (also known as rapamycin) with pulsed dye laser (PDL) treatments.
PDL is the gold standard treatment option for CMs and lightens the color of the birthmark. The laser only goes through the top layer of skin, so deeper blood vessels are not treated.
Many treatments with PDL are needed to get the best results and are typically spaced 4–12 weeks apart. Once a good result from laser treatment is achieved, some maintenance or “touch-up” treatments will be needed after several years because the color may darken again over time.
PDL can lighten most CMs to 50 to 90 percent of their original color. Very few will disappear completely with laser treatment.
PDL gives the best results when treating the head and neck. Response on the arms and legs is often not as good, and more treatments are often needed to get the best possible results.
A topical numbing cream (topical anesthetic) can be applied to the area before laser treatment.
Some young children with large CMs need brief general anesthesia for PDL treatments. Most small- and medium-sized CMs can be treated in the office by experienced doctors without the need for sedation.
Surgery may be recommended if there is an overgrowth of tissue, such as extra bone or skin. This is not common. When it happens, it is usually in adults or associated with another, deeper, vascular malformation.
If there is an overgrowth of fat, this can sometimes be removed with a procedure called suction-assisted lipectomy. For overgrowths on the face, surgery can help improve symmetry and appearance.