Clinical Collaboration and Teamwork
The Clinical Collaboration and Teamwork award is presented to the physician, nurse and/or team who engages colleagues in shared decision-making, fostering cooperation and open communication.

Johns Hopkins Howard County Medical Center
Andrew Demidowich, M.D.
Endocrine and Inpatient Diabetes Management Service
When Andrew Demidowich started at Johns Hopkins Howard County Medical Center, he reviewed patient outcomes data and realized there was a need to change the culture around diabetes management. “Dr. D” began holding meetings with the frontline nurses to start the re-education process. He attended HCGH's Nursing Practice Council to present his findings and to talk about the motivated nurses who heard his call for help and responded. A true patient advocate and nursing partner, he realizes that culture changes take time, but encourages the team to think of innovative ways to make a difference more quickly using subtle modifications.

Johns Hopkins All Children’s Hospital
Deanna Green, M.D., and the Cystic Fibrosis Care Center Team
The multidisciplinary cystic fibrosis care team coordinates care for 180 patients with CF as well as 55 patients who come through the center for laboratory and genetic testing as newborns. It includes members from nursing, respiratory care, physical therapy, nutrition, social work and mental health. This year, the team started its own quality improvement initiatives to better educate inpatient staff members and to help transfer knowledge to those who do not frequently interact with patients from the center. With input from all disciplines, the patient population treated by the team has maintained lung function above the 95th percentile for the past six years.
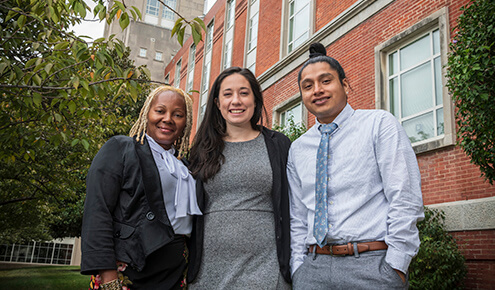
Johns Hopkins Bayview Medical Center
Megan Buresh, M.D., and the Comprehensive Care Practice Community Health Workers
In 2017, the Comprehensive Care Practice and Division of Addiction Medicine at Johns Hopkins Bayview established a specialized Community Health Worker (CHW) Program, which links CHWs who have lived experience with patients contemplating recovery or in recovery to assertively engage, offer support and mitigate barriers to care. The CHWs provide tangible resources outside of medical treatment, including access to housing, job opportunities and financial support for medical expenses, as well as assertive facilitation of medical care. The CHWs are embedded in the Comprehensive Care Practice, a primary care setting that manages substance use disorders and chronic illnesses in close coordination with a care management team and advanced practice providers.
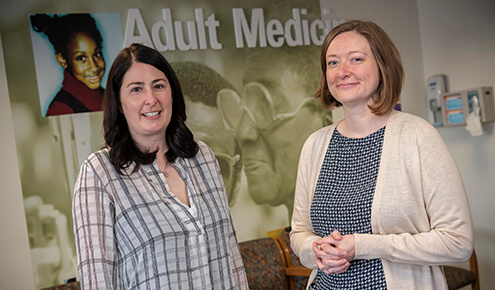
Johns Hopkins Community Physicians
Kate Rediger, C.R.N.P., Laura Harding-Fukushima and the Trauma-Informed Care Work Group
Acknowledging that trauma affects both patients and staff members at East Baltimore Medical Center (EBMC), Kate Rediger organized a trauma-informed care work group. She created this work group to improve the care of vulnerable patients who experience trauma and PTSD on a daily basis and to address the trauma and secondary trauma that staff at EBMC face. By doing so, the group seeks to improve health equity for vulnerable patients, decrease burnout and increase joy in medicine for staff members and providers.

The Johns Hopkins Hospital
Albert Wu, M.D., Cheryl Connors, R.N., Matt Norvell and the RISE Team
The Resilience in Stressful Events (RISE) team is composed of volunteers who serve the entire campus 24/7. They work collaboratively to provide support to employees at a minute’s notice and support each other daily. Selfless and without hierarchy, this multidisciplinary team exhibits mutual respect among team members and to all they serve regardless of discipline. RISE has served over 1,000 employees at The Johns Hopkins Hospital and, anecdotally, has contributed to the well-being of employees and saved the life of at least one colleague.

Sibley Memorial Hospital
Margaret Showel, M.D., and the Hematologic Malignancy Team
A fierce patient advocate, Margaret Showel works collaboratively with various teams throughout Sibley Memorial to deliver exceptional care to her hematology/oncology patients, who are often the most vulnerable and delicate patient population at Sibley. Dr. Showel has engaged with the emergency department to optimize the care of the growing oncology population, and she has worked tirelessly to educate all providers on patient-centered care related to this specific group of patients.

Suburban Hospital
Structural Heart Disease Program
The Suburban Structural Heart Disease Program works in close collaboration with and under the umbrella of the Johns Hopkins Structural Heart Disease Program based in Baltimore. The multidisciplinary team provides high-quality care to patients with severe valvular heart disease and other complex cardiovascular disease using minimally invasive, catheter-based approaches — especially transcatheter aortic valve replacement (TAVR) — and other relatively new and innovative techniques and surgical approaches. Most of the program’s patients are elderly, and conventional surgical approaches are considered too risky or unfeasible. This team has worked arduously to establish a means for these patients to be evaluated and treated locally, starting with the establishment of a clinic at Suburban Hospital to conduct TAVR procedures and including extensive efforts in comprehensive evaluation, procedural planning and execution.
