Lumbar Puncture
A lumbar puncture (LP) or spinal tap may be done to diagnose or treat a condition. For this procedure, your healthcare provider inserts a hollow needle into the space surrounding the spinal column (subarachnoid space) in the lower back to withdraw some cerebrospinal fluid (CSF) or inject medicine.
CSF is a clear fluid that bathes and cushions the brain and spinal cord. It is continuously made and reabsorbed in the brain. CSF is made up of cells, water, proteins, sugars, and other substances that are essential to maintain balance in the nervous system.
Why might I need a lumbar puncture?
A lumbar puncture may be done for various reasons. The most common reason is to remove a small amount of CSF for testing. This can help in the diagnosis of various disorders. The fluid is tested for red and white blood cells, protein, and glucose (sugar). The clarity and color of the fluid are also checked and it is tested to see whether bacteria, viruses, or abnormal cells are present. Excess CSF may also be removed in people who have an overproduction or decreased absorption of the fluid.
A lumbar puncture procedure may be helpful in diagnosing many diseases and disorders, including:
-
Meningitis. An inflammation of the membrane covering the brain and spinal cord. The inflammation is usually the result of a viral, bacterial, or fungal infection.
-
Encephalitis. An inflammation of the brain that is usually caused by a virus.
-
Certain cancers involving the brain and spinal cord
-
Bleeding in the area between the brain and the tissues that cover it (subarachnoid space)
-
Reye syndrome. A sometimes fatal disease that causes severe problems with the brain and other organs. Although the exact cause of the disease is not known, it has been linked to giving aspirin to children. It is now advised not to give aspirin to children during illnesses, unless prescribed by your child's healthcare provider.
-
Myelitis. An inflammation of the spinal cord or bone marrow.
-
Neurosyphilis. A stage of syphilis during which the bacteria invades the central nervous system.
-
Guillain-Barré syndrome. A disorder in which the body's immune system attacks part of the nervous system.
-
Demyelinating diseases. Diseases that attack the protective coating that surrounds certain nerve fibers - for example, multiple sclerosis or acute demyelination polyneuropathy.
-
Headaches of unknown cause. After evaluation and head imaging if necessary, a lumbar puncture may be done to diagnose certain inflammatory conditions that can result in a headache.
-
Pseudotumor cerebri (also called idiopathic intracranial hypertension, or IIH). In this condition,pressure within the subarachnoid space is elevated for reasons that are not clear. A lumbar puncture is only done in this condition after evaluation and head imaging.
-
Normal pressure hydrocephalus. A rare condition affecting mainly older people in which there is a triad of loss of urinary control, memory problems, and an unsteady gait. A lumbar puncture is done to see if the pressure of the CSF is elevated or not.
In addition, a lumbar puncture may be used
to measure the pressure of the CSF. The healthcare provider uses a special tube
(called a manometer) to measures the pressure during a lumbar puncture.
Finally, a lumbar puncture may be done to inject medicine directly into the spinal cord. These include:
- Spinal anesthetics before a surgical procedure
- Contrast dye for X-ray studies - for example, myelography
- Chemotherapy drugs used to treat cancer
Your healthcare provider may have other reasons to recommend a lumbar puncture.
Pseudotumor Cerebri | Ashley's Story
After visiting 30+ physicians, Ashley was diagnosed with the rare condition known as pseudotumor cerebri. She and her family turned to the experts at Johns Hopkins who worked as a team to implant a stent, a new approach to treating this condition that is typically treated with a shunt.
What are the risks of a lumbar puncture?
Because this procedure involves the spinal cord and brain, the following complications may occur:
- A small amount of CSF can leak from the needle insertion site. This can cause headaches after the procedure. If the leak continues, your headache can be severe.
- You may have a slight risk of infection because the needle breaks the skin’s surface, providing a possible way for bacteria to enter the body.
- Short-term numbness of the legs or lower back pain may be experienced.
- here is a risk of bleeding in the spinal canal.
There may be other risks depending on your specific medical condition. Be sure to discuss any concerns with your healthcare provider before the procedure.
How do I prepare for a lumbar puncture?
If you are having a lumbar puncture at Johns Hopkins Hospital or Bayview Medical Center, a neuroradiologist or radiology nurse will contact you by phone two or three days prior to your lumbar puncture to discuss the procedure and answer any questions you may have.
Please inform the neuroradiology physician if:
- You are on antibiotics - you may need to wait to do the procedure if currently on antibiotics for an in infection in your blood. If you have an active infection or fever, your procedure may need to be rescheduled.
- You are allergic to any local anesthetics (lidocaine)
- There is any chance that you could be pregnant
- You are on anticoagulant therapy (blood thinners)
PRECAUTIONS: If you are pregnant or think you might be pregnant, please check with your doctor before scheduling the exam. Other options should be discussed with you and your doctor.
CLOTHING: You may be asked to change into a gown. A gown will be provided for you. However, the procedure may also be done while you remain in your clothes from home. For this reason, try to wear non-restrictive, comfortable clothing and slip on shoes if possible. Please remove all piercings and leave all jewelry and valuables at home
EAT/DRINK: Try to increase your fluid intake (such as water and juice) for the two days leading up to your procedure unless a medical condition does not allow you to safely do so. If you are not sure if it is safe for you, contact your primary care provider or referring provider.
However, on the day of the procedure, do not eat for three hours before the procedure. You may have liquids and can take your usual medications unless previously advised to hold certain medications in preparation for the lumbar puncture.
MEDICATION: All patients can take their prescribed medications as usual unless instructed to hold certain medications such as blood thinners. Please bring a current list of your medications and allergies with you.
TRAVEL: You must have an adult driver accompany you so they can drive you home after the procedure. This is for your safety and comfort.
- Arrive one hour prior to the scheduled procedure time for check-in and to be prepped for the procedure.
- Please note: You will be unable to drive for 24 hours after the procedure. If you are taking a cab or using public transportation, you need to bring a friend or family member to accompany you after the procedure to your home or hotel. A cab or public transportation driver is not considered an escort.
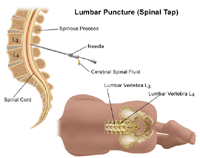
What happens during a lumbar puncture?
A lumbar puncture procedure may be done on an outpatient basis or as part of your stay in a hospital. Procedures may vary depending on your condition and your doctor's practices. Some healthcare providers may prefer to do this procedure at the bedside or may opt to have it done using a type of live X-ray called fluoroscopic guidance.
Generally, a lumbar puncture follows this process
- You will remove any clothing, jewelry, or other objects that may interfere with the procedure
- You will be given a gown to wear.
- You will be reminded to empty your bladder prior to the start of the procedure.
- During the lumbar puncture you may lie on the exam table on your side with your chin tucked to your chest and knees tucked to your abdomen. Or, you may sit on the edge of an exam table with your arms draped over a table positioned in front of you. In either position the back is arched, which helps to widen the spaces between your vertebrae.
- Therefore, your back will be cleansed with an antiseptic solution and draped with sterile towels. The healthcare provider will wear sterile gloves during the procedure.
- The provider will numb the skin by injecting a local anesthetic. This injection may sting for a few seconds, but makes the lumbar puncture less painful.
- The hollow needle will be inserted through the numbed skin and into the space where the CSF is located. You will feel some pressure while the needle is inserted. You must remain absolutely still during the insertion of the needle.
- The CSF will begin to drip out of the needle and a small amount, about one tablespoon, will be collected into test tubes.
- If the provider needs to inject medicine into the spinal canal, it will be given through the same needle after the CSF is collected.
- When the procedure is done, the needle will be removed and a bandage will be placed over the injection site. The test tubes will be taken to the lab for testing
- Tell the healthcare provider if you feel any numbness, tingling, headache, or light-headedness during the procedure.
You may have discomfort during a lumbar puncture. Your healthcare providers will use all possible comfort measures and complete the procedure as quickly as possible to minimize any discomfort or pain.
What happens after a lumbar puncture?
This helps reduce the incidence of a headache. You will be allowed to roll from side to side as long as your head is not elevated. If you need to urinate, you may need to do so in a bedpan or urinal during the time that you need to stay flat.
You will be asked to drink extra fluids to rehydrate after the procedure. This replaces the CSF that was withdrawn during the spinal tap and reduces the chance of developing a headache.
After recovery, you may be taken to your hospital room or discharged to your home. If you go home, usually your healthcare provider will advise you to rest for the remainder of the day
Once you are at home, notify your provider of any abnormalities, such as:
- Numbness and tingling of the legs
- Drainage of blood or pain at the injection site
- Inability to urinate
- Headaches
If the headaches persist for more than a few hours after the procedure, or when you change positions, contact the neuroradiology team with the phone number provided on your discharge instructions.
You may be instructed to limit your activity for 24 hours following the procedure.
Your healthcare provider may give you other specific instructions about what you should do after a lumbar puncture.