Johns Hopkins Howard County Medical Center is a private, not-for-profit, community health care provider, governed by a community-based board of trustees. Since its founding in 1973, the original 59-bed, short-stay hospital has grown into a comprehensive acute care medical center with 262 licensed beds. We specialize in women’s and children’s services, surgery, cardiology, oncology, orthopedics, gerontology, psychiatry, emergency services and community health education.
Our mission, "Provide the highest quality care to improve the health of our entire community through innovation, collaboration, service excellence, diversity and a commitment to patient safety" is carried through in everything we do.
Johns Hopkins Howard County Medical Center
We have been at the center of caring for our community since 1973. Learn more about some of our key services.
Historical Highlights
-
1968 – The Johns Hopkins Hospital and Connecticut General Life insurance Company team up to create one of the first health maintenance organizations.
1970 – The groundbreaking for the new Columbia Medical Center takes place.
1971 – Columbia Hospital & Clinics Foundation is formed.
1973
July 9 – The Columbia Hospital and Clinics Foundation, Inc., opens its doors as a 59-bed, short-stay hospital.
July 17 – Columbia Hospital and Clinics Foundation is fully operational. The hospital has 75,000 square feet, including: emergency facilities, a three-bed coronary unit, a ten-bassinet nursery, operating rooms and delivery suites, and 59 general patient beds. The hospital initially serves anyone in need of emergency care, patients of Howard County physicians with staff appointments to the hospital and members of the Columbia Medical Plan.
September 13 – The Columbia Hospital and Clinics Foundation is officially dedicated.
1974 – Columbia Hospital and Clinics Foundation changes ownership and control.
Columbia Hospital and Clinics Foundation becomes independent of Johns Hopkins and changes its name to Howard County General Hospital, a private, nonprofit hospital governed by a board of trustees representing the community it serves. Patients with all types of insurance can be admitted.
1975 – The hospital applies to the Maryland Comprehensive Health Planning Agency asking to construct a 120-bed addition. in 1976.
1976 - The Howard County General Hospital Capital Fund, Inc., the predecessor of the Howard Hospital Foundation, is established and raises $1.7 million of the $8.8 million needed, and construction begins for the hospital addition.
1977 - Work begins on a two-story, multispecialty medical office building on hospital property, known as the Medical Arts Building.
1978 - HCGH opens a 56-bed satellite acute care facility at Lorien Nursing home to serve as an interim expansion to ensure hospital capacity meets community needs.
1980 - The North Wing expansion opens adding 120 beds. The expansion includes improved Labor and Delivery rooms, a pharmacy, dietary services as well as more beds to the Critical Care Unit and a 21-bed step-down Intermediate Care Unit. The newborn nursery is expanded and the entire third floor of the hospital is dedicated to the treatment of maternity and gynecology patients.
1981- An eight-bed pediatric cluster opens on the second floor of the new North Wing.
1986 - Construction begins on the second building expansion to include an outpatient testing center.
1987 - Howard Health System is created as a parent company to HCGH to plan and coordinate hospital and health services for Howard County residents.
1988 – The ribbon cutting for new South Wing takes place. The $28 million construction and renovation project provides 72 new medical/surgical beds, a new main entrance and a cafeteria.
1989 - The Cardiac Rehabilitation Program begins, led by David S. Jackson, M.D., a cardiologist with Maryland Primary Care Physicians.
1990 - Victor A. Broccolino becomes president and CEO of HCGH.
A six-bed Special Care Nursery opens to provide care to high-risk infants by full-time neonatologists.
1992 - The Capital Fund is renamed the Howard Hospital Foundation to better reflect the breadth of its fundraising mandate.
A 6,500 square foot addition is built to accommodate the Magnetic Resonance Imaging (MRI) Center.
1993- The First Annual Symphony of Lights is held in Columbia.
1994 - HCGH initiates one of the most advanced, freestanding regional oncology centers on the East Coast at the Central Maryland Oncology Center. The center is a joint initiative between HCGH and the University of Maryland Medical Center.
1996 - The Ambulatory Care Center opens housing a multispecialty outpatient surgical facility.
The Central Maryland Heart Center opens. The county's first cardiac catheterization laboratory is a joint venture between Johns Hopkins Medicine and HCGH.
HCGH, through a contract with the Johns Hopkins University School of Medicine, initiates a maternal fetal medicine service at the hospital to care for women at high-risk during their pregnancies. Johns Hopkins physicians provide consultation services to local obstetricians and manage the Center for Maternal Fetal Medicine.
1997 - A comprehensive pediatric unit opens, staffed by Johns Hopkins pediatric specialists, who provide emergency, observation and inpatient services.
The 13-bed Chest Pain Unit (now called the Observation Unit) is opened on the first floor of the hospital.
The 4 South nursing unit opens to serve oncology patients. -
1998 - After a two-year planning period, the Board of Trustees votes to enter a strategic partnership to become a member of Johns Hopkins Medicine and the first community hospital in the Johns Hopkins Health System. The Horizon Foundation is formed through the merger and capitalized with a $66 million gift from HCGH.
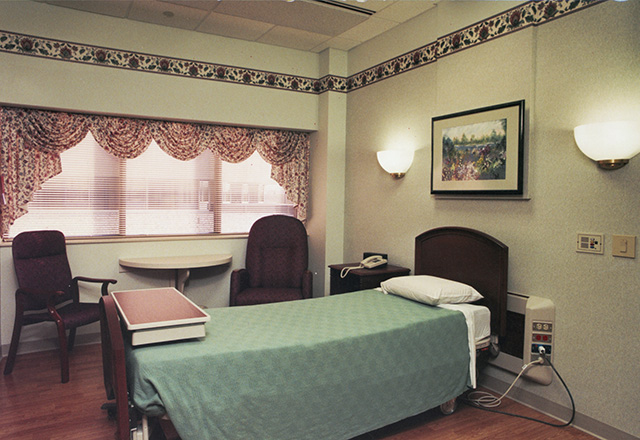
The new Maternal Child Unit opens, featuring nearly all private rooms for new parents.
The Claudia Mayer Cancer Resource and Image Center opens, providing free information and support for cancer patients, their families and caregivers.
1999 - The Special Care Nursery is upgraded to a Level III Neonatal Intensive Care Unit (NICU) and staffed by Johns Hopkins neonatologists.
2000 - The Howard Hospital Foundation launches its Master Facility Campaign, a four-year capital campaign to help fund the $34 million project to construct a new Emergency Department, Intensive Care Unit and obstetrics facilities.
2001 - A new 16-bed Intensive Care Unit (ICU) opens as part of the hospital’s expansion and renovation.
The Johns Hopkins Wilmer Eye Institute, an internationally-renowned eye institution, opens a practice on the campus of HCGH.
2002 - A state-of-the- art Emergency Department opens, triple in size of the former Emergency Department, with services provided by Johns Hopkins Emergency Medicine physicians.
HCGH purchases a 10-acres of land in anticipation of a growing demand for health care services in the county - increasing the campus size by 50 percent. Seven years later, the Medical Pavilion at Howard County opens on the land.
The new Labor and Delivery and Neonatal Intensive Care Units (NICU) open adjacent to the Maternal Child (Postpartum) unit providing contiguous maternal child facilities in the West Wing of the hospital.
2003 - The Center for Wound Healing opens to treat patients with non-healing and chronic wounds.
Intensivist medicine is introduced in the Intensive Care Unit (ICU), providing round-the-clock coverage by intensivist physicians.
HCGH was granted approval by the Maryland Health Care Commission to provide this primary percutaneous coronary intervention (PCI) in the hospital. This life-saving procedure, which opens clogged arteries, helps patients experiencing certain types of heart attacks called STEMIs.
2005 - HCGH adds cardiac electrophysiology treatment with the addition of Johns Hopkins arrhythmia specialty physicians—cardiologists with added expertise in abnormal heart rhythms— to the staff.
2006 - The Center for Maternal Fetal Medicine is staffed and managed by Johns Hopkins specialists, providing a team approach to perinatal care and management of high-risk pregnancies.
2007 - The Campus Development Plan begins, a multiyear project to provide the hospital with a brand new five-level Patient Pavilion that houses inpatient floors with all private rooms and offers new outpatient space.
The Behavioral Health Unit opens in the Emergency Department, providing a separate, secure and comfortable treatment space for patients presenting with mental health conditions.
2008 - HCGH becomes a state-certified primary stroke center.
2009 - The Medical Pavilion at Howard County opens – a five-level, 167,000 sq. ft. building housing medical practices, the Johns Hopkins Laboratory, Johns Hopkins Outpatient Pharmacy, Claudia Mayer Cancer Resource Center, Central Maryland Radiation Oncology and HCGH Wellness Center.
The new five-story Patient Pavilion opens with all private rooms and includes the new The Bolduc Family Outpatient Center.
2012 – The Breast Center at HCGH opens, under the leadership of Lisa K. Jacobs, M.D., a Johns Hopkins surgical oncologist.
2013 – The Johns Hopkins Center for Sleep opens at HCGH directed by Johns Hopkins sleep specialists Charlene Gamaldo, M.D., and Rachael Salas, M.D.
2014 –Vic Broccolino, longest-serving president and CEO of HCGH, retires.
Steve Snelgrove becomes HCGH president.
The Health Care and Surgery Center building is renamed the Dr. Sanford A. Berman Dr. Kay Ota-Berman Pavilion in recognition of their $5 million donation. This is the largest private donation in the history of both Howard County General Hospital and Howard County at large. -
2018 - The Armstrong Institute for Patient Safety and Quality expands to HCGH, fortifying the hospital’s ability to provide the highest quality and safest care to the community it serves.
2019 - The Johns Hopkins Vein Center in Columbia opens staffed by Johns Hopkins vascular surgeons.

The Johns Hopkins Musculoskeletal Center opens adjacent to HCGH staffed by Johns Hopkins orthopedic specialists. The Johns Hopkins Rehabilitation Network at Columbia offers physical, occupational and speech therapy.
2020 – New 50,000 sq. ft. addition opens, providing a new pediatric and adult emergency room entrance as well as expanded and improved observation and psychiatric units.
HCGH begins offering elective percutaneous coronary intervention (PCI) services (formerly known as angioplasty and stenting) to open narrowed heart arteries. This allows patients the ability to receive outpatient interventional catheterization procedures in their community.
March: COVID-19 strikes. Faced with an overwhelming crisis unlike anything we had ever experienced, we had to change the way we work, implement new protocols, policies and procedures at lightning speed, and practically rebuild hospital rooms and move units entirely.
2021– Shafeeq Ahmed, M.D., becomes President and CEO of HCGH.
2022 – Specialty services from Johns Hopkins physicians, such as women’s gynecologic oncology surgery and robotic surgery, expand on the medical campus.
2023 – Primary care expands in Howard County through Johns Hopkins Community Physicians.Howard County General Hospital’s name changes to Johns Hopkins Howard County Medical Center. The medical center offers the same services under the new name, with the goal of further expanding Johns Hopkins specialty care in the future.
-
In March 2020, the world shut down. The COVID-19 pandemic caused business, schools and government offices to close their doors. At Howard County General Hospital, our community and patients relied on us to keep our doors open to care for both COVID and non-COVID patients.
From the first announcement of the pandemic, HCGH’s leadership team began preparing for the worst, initiating our emergency response. Almost every employee in the hospital had a role in the crisis situation. Our physical plant staff set to work converting patient rooms to negative pressure and building walls to separate COVID patient care areas.
The Incident Command team worked closely with Johns Hopkins Medicine Incident Command to identify and implement the best practices for patient care while protecting patients and staff from infection. It was critical for staff to follow the guidance for properly wearing personal protective equipment, while conserving the equipment so that we had sufficient inventory.
COVID-19 was a new virus that caused such severe conditions that clinicians had to learn new methods of care. For example, the physical therapy team worked with nursing to put patients in a prone position to allow their damaged lungs to better expand.
Staff in various non-clinical positions pivoted and worked outside of their normal sphere in areas that needed assistance. Occupational therapists helped serve patient meals, Cardiac Rehab staff set up and operated a COVID testing facility, managers helped clean the hospital, deliver inventory and run specimens from patient units to the Laboratory.
After the initial intensity of the first few months, HCGH settled into a new normal of operating in a pandemic era. While we experience some spikes in COVID patients from time to time, we are better prepared to meet the challenges.
“Our response to the pandemic has proven that our staff are incredible, selfless and, above all, resilient,” said Shafeeq Ahmed, M.D., MBA, FACOG, HCGH president. “It has been said that working at HCGH is like working with your family. We came together as one to meet the needs of our community and stay true to our mission of providing exceptional patient care.”
While the COVID-19 pandemic has been difficult, HCGH has risen to the challenge and is better prepared for future pandemics or emergencies.
Facts about Johns Hopkins Howard County Medical Center
Fiscal Year 2024 Utilization Statistics
-
73K Emergency Room Visits
For patients that were evaluated and treated
-
20K Patients
Admitted to or observed in the hospital
-
8K Surgeries
2,682 performed in the hospital; 5,489 performed as outpatient procedures
-
2,476 Babies Delivered
In our Labor and Delivery unit
-
26K Outpatient Services
Provided to patients including laboratory / excluding outpatient surgery
-
1K People
Screened through our health promotions and wellness programs