Diagnosing and Treating Peripheral Arterial Disease
What is Peripheral Arterial Disease?
Peripheral arterial disease (PAD) is a narrowing of the arteries outside of the heart and brain. The term is most frequently used to describe the narrowing of arteries to the lower limbs. It is estimated that 10 to 14 million people in the U.S. suffer from this condition, and it is equally prevalent among men and women.
“Peripheral vascular disease refers to all of the blood vessels outside the heart, diseases of the arteries and diseases of the veins,” says Dr. Kerry J. Stewart, director of Clinical and Research Exercise Physiology at Johns Hopkins Bayview Medical Center. “In cardiology, what we’re most likely to deal with are diseases of the arteries that supply blood to the lower limbs.”
The most common disease of the arteries is atherosclerosis, a buildup of plaque that could eventually obstruct blood flow to the muscles and organs. When it affects the arteries of the brain, this could lead to stroke. When the blockage is in the legs, it could lead to peripheral arterial disease.
Symptoms of Peripheral Arterial Disease
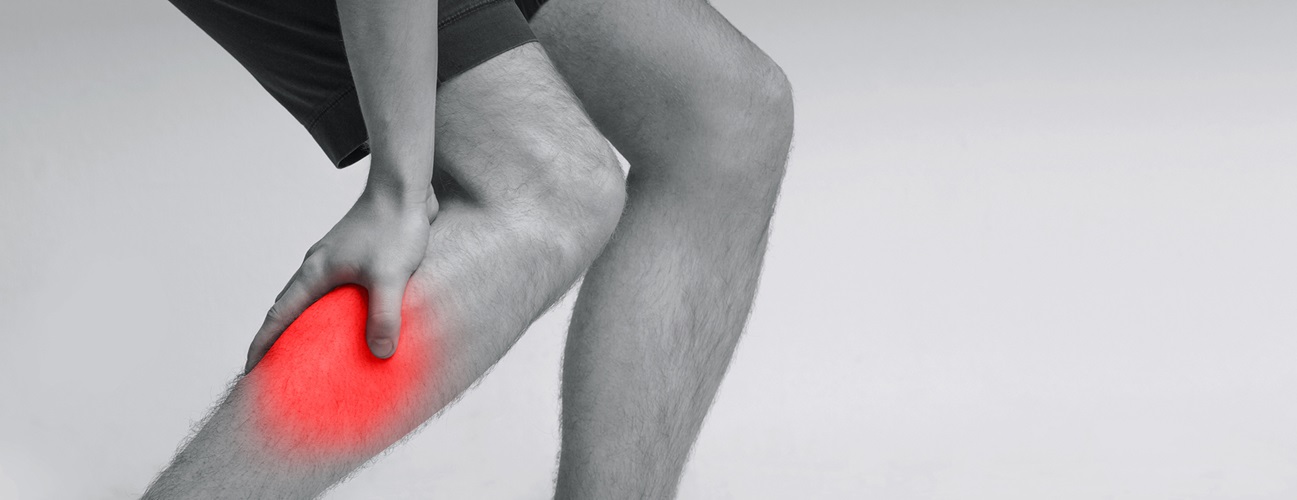
Because the arteries that feed the legs are narrowed by plaques, it causes a lack of blood flow, creating a condition known as ischemia. Ischemia occurs when the demand for oxygen is greater than the supply.
The most common symptom of this interrupted blood flow is intermittent claudication – a cramping in the legs and buttocks that flares up when you walk and subsides when you stop. Intermittent claudication occurs in only about 40 to 50 percent of patients with PAD. Other symptoms may include numbness or coldness in the feet, and a loss of hair around the ankles. For reasons that are unknown, patients can have PAD but not have these symptoms.
Among patients who do suffer pronounced symptoms such as claudication, a domino effect can occur:
Cramping and pain while walking can lead to a more sedentary lifestyle; which can lead to burning fewer calories and weight gain; which can lead to the increase of LDL (low density lipoprotein) cholesterol, blood pressure, and several other risk factors for heart disease.
Risk Factors and Diagnosis
Peripheral arterial disease shares many risk factors with heart disease. So it’s important to be screened if you’re already at high risk for heart disease and have any of the following risk factors:
- smoking
- diabetes
- high cholesterol
- high blood pressure
- obesity and physical inactivity
Cramping and pain in the legs can have other causes, such as sciatica, arthritis, and nerve damage. And you can have peripheral arterial disease without noticeable symptoms. So if you’re at generally higher risk for heart disease, it’s recommended that you see your physician to sort out symptoms and risk factors, and test for peripheral arterial disease.
There is a simple test called the ankle-brachial index (ABI). It compares blood pressure in the arm to blood pressure in the leg. Blood pressure should be uniform throughout the whole body, so if pressure is higher in the arm than the leg, it means there’s less blood flowing to the legs, which can indicate blockage in the arteries.
Treating Peripheral Arterial Disease
Because peripheral arterial disease is atherosclerosis, an individual who has PAD is also at high risk for heart disease or stroke, which are also caused by atherosclerosis. For this reason, PAD is a risk factor for these more life-threatening conditions. Therefore, the treatment for PAD includes aggressively managing heart attack and stroke risk factors:
- quitting smoking
- controlling diabetes and blood pressure
- lowering low-density lipoprotein (LDL) cholesterol and triglycerides
- taking anticoagulants to prevent blood clots
- incorporating medically supervised exercise into your daily life
“The most effective therapy for improving the symptoms of mild to moderate forms of peripheral artery disease is exercise training,” stresses Stewart. “Five to ten percent of patients have to deal with critical leg ischemia that causes severe enough pain to require bypass surgery or some other surgical means of restoring blood flow. But the vast majority of people should be offered an exercise program.”
Johns Hopkins Women's Cardiovascular Health Center